Breast reduction, also called reduction mammaplasty, is a well established procedure that can relieve physical discomfort linked with heavier breasts and make everyday activities more manageable. For many people across Newcastle and the Hunter region, it can reduce neck and shoulder strain, rashes beneath the breast fold, and limitations with exercise. The operation itself is only one part of the journey. What happens afterwards matters just as much. Recovery is a sequence of planned steps where swelling settles, sensation changes gradually improve, and activity returns in a measured way. This guide explains what Recovery after Breast Reduction in Newcastle typically involves, how long key milestones may take, and the simple actions that support healing. It is focused on practical detail and realistic expectations.
Dr Yezdi Mistry is a Specialist Plastic Surgeon based in Charlestown. His practice is built around careful preoperative planning, thorough consent, and attentive follow up. Patients receive individual advice that reflects their health, the specifics of their operation, and the pace at which they are healing. The information below describes common patterns while recognising that each person’s recovery is individual.
Recovery after breast reduction progresses in phases. The first week centres on comfort, wound care, and gentle walking around the home. Weeks two to four usually bring decreasing swelling and a return to light daily tasks. Between two and six months most people resume a wide range of activities, with attention to scar care and sensible load management. Final settling takes longer. The appearance and feel of the breasts and the look of the scars continue to evolve for 12 to 18 months as collagen remodels and the skin envelope adjusts to the new volume.
During surgery, excess breast tissue and skin are removed, the remaining tissue is reshaped, and the nipple and areola are repositioned to suit the new breast footprint. The incision pattern and the amount of reduction influence the early course of healing. Larger reductions often need a longer period for swelling to subside. Smaller reductions may settle more quickly. These considerations are discussed in consultation so your postoperative plan reflects your operation.
Good preparation helps. Arrange assistance at home for the first fortnight, particularly if you have young children or caring responsibilities. Prepare simple meals, set up a comfortable sleeping position with pillows for upper body support, and choose front opening tops that do not require lifting arms overhead. These small steps make the early period smoother.
The first 24 to 72 hours usually bring predictable fullness and a sense of tightness across the chest. A supportive surgical bra is fitted to limit tissue movement and reduce swelling. Some patients have small drains for a short time to remove fluid. Dressings protect the incisions and stay in place until your first review unless you are advised otherwise.
Pain is often described as pressure rather than sharp pain and is managed with prescribed medication. Short, frequent walks around the house help circulation, reduce stiffness, and lower the risk of clots. Keep arm movements within a comfortable range. Reaching to high shelves, pushing through the arms to get out of deep chairs, and carrying even moderate loads is avoided. Sleep on your back with your upper body slightly elevated. This position reduces strain on the chest and helps swelling settle.
It is normal for the breasts to sit higher and feel firmer at this stage. Bruising and swelling can make them look fuller in the upper pole. Shape in the first week never represents the final outcome. If you notice increasing redness, escalating pain that does not respond to medication, sudden swelling on one side, a fever, or unusual discharge from a wound, contact Dr Mistry’s rooms for review.
By the second week most people feel steadier on their feet and more comfortable. Bruising fades from purple to yellow, and swelling becomes less tense. Any drains are usually removed within a few days of surgery and sutures that require removal are taken out according to the method used. The supportive garment remains important and is generally worn day and night for several weeks. It reduces shear forces across healing tissues and makes movement more comfortable.
Light household tasks are often acceptable during this period. Short walks outdoors are encouraged, along with gentle stretching that does not place load through the chest. Desk based work may be possible at two to three weeks depending on how you feel and the nature of your job. Roles that involve lifting, repetitive arm use, or overhead work typically require a longer pause and a staged return plan agreed at review.
Sensation changes are common. Temporary numbness around the nipple or the lower breast skin and intermittent tingling reflect nerve recovery. Mild itching around the incision lines is part of normal healing. If sensitivity becomes bothersome, the team can suggest simple desensitisation strategies. Regular follow up appointments are a practical anchor during these weeks. Dr Mistry checks wound progress, confirms swelling is trending down, and offers specific guidance on showering, garment use, driving, and very gentle self massage if suitable.
By the second month much of the swelling has resolved. The breasts begin to soften and to sit more naturally on the chest wall. The lower pole rounds out, and the upper fullness looks less pronounced. Scars that were pink or slightly raised begin to flatten as collagen remodels. Scar care with silicone products and consistent sun protection is often recommended. In Australian conditions it is important to protect incision lines from the sun for at least a year as ultraviolet exposure can darken scars.
Exercise is reintroduced in stages. Many patients restart low impact aerobic activity such as walking or stationary cycling around six weeks, progressing based on comfort and medical advice. Upper body resistance work needs caution. Press ups, heavy pushing or pulling, and overhead lifts place load across healing tissues and should wait until the surgeon confirms readiness. A simple rule helps. Add one new demand at a time, monitor your response for 24 to 48 hours, and only progress when there is no increase in soreness or swelling.
Daily life often feels easier in this phase. Neck and shoulder pressure related to breast weight usually lessens, straps sit more comfortably, and clothing options broaden. This is also when emotional adjustment becomes clearer. Some people notice immediate relief. Others become gradually aware of practical benefits like improved posture or greater ease with exercise. Both experiences are normal. Keep talking with the team at review if you have questions about shape, sensation, or activity.
Nutrition continues to matter. Balanced meals with adequate protein support tissue repair. Hydration helps skin and scar health. If you smoke, complete cessation is strongly recommended, since nicotine reduces skin blood flow and increases the chance of delayed healing. Alcohol is kept modest, especially while taking prescribed medication. These simple measures support good recovery.
Beyond six months the breasts feel softer and more natural to touch. Small irregularities gradually even out as the internal scar tissue matures. The breast mound position becomes more stable. Scars continue to fade and usually become paler than the surrounding skin. The timeline for this improvement varies. Genetics, skin type, tension across the incision, and the consistency of scar care all play a part. Many people see ongoing gains into the second year.
If a scar area becomes thick or itchy, options such as silicone therapy, massage, taping, or targeted in clinic treatments can be discussed. Sun protection remains worthwhile even after scars appear faint. Long term results also reflect general health. Large changes in weight, pregnancy, some medications, and natural ageing affect all breast tissue over time. If you notice late changes that you would like to discuss, book a review once healing is mature.
There is no single recovery timeline that suits everyone. Overall health, nutrition, sleep quality, and stress levels influence tissue repair. Smoking slows skin blood flow and is a major risk for wound problems. Stopping well before and after surgery is strongly encouraged. Medical conditions such as diabetes or connective tissue disorders may require additional precautions. These are addressed during planning so that risks are sensibly managed.
The size of the reduction and the specific surgical pattern also matter. Larger reductions and operations that require extended reshaping often involve a longer period of swelling and garment use. Smaller reductions or liposuction assisted steps may settle more rapidly. Neither approach is inherently preferable. Technique is chosen to match your anatomy, symptoms, and aims.
You can influence recovery through consistent self care. Wear the recommended garment as directed. Keep incisions clean and dry as advised. Attend scheduled reviews. Avoid heavy lifting until cleared. If questions arise at home, do not guess. Contact the rooms so that a clinician can guide you.
Emotional wellbeing is part of recovery. It is reasonable to feel a mixture of relief, fatigue, and curiosity as you adapt to a different breast size and shape. Give yourself time and set simple milestones such as walking comfortably by the end of week one, returning to light duties at two to three weeks if appropriate, and discussing structured exercise at your next review rather than rushing ahead.
Right after surgery the breasts sit higher and feel firm. Swelling makes the upper pole appear fuller. Over the next several weeks the lower breast pole develops a gentle curve and the upper area softens. Early asymmetry is common because swelling is rarely identical on both sides. This usually evens out as healing continues.
Sensation around the nipple and lower breast often changes. Some people notice reduced sensitivity, others notice tingling. The majority of these changes improve over several months as nerves recover. In a smaller number of cases altered sensation can persist. This possibility is part of the consent discussion before surgery so expectations are realistic.
Scars are a natural consequence of moving and reshaping skin. Initially they are fine lines that appear pink. They can look a little more noticeable before they look better while collagen is remodelling. Regular silicone therapy, gentle massage when advised, and sun protection support an even, flat scar in most cases. If you are prone to thicker scarring, stay in close contact with the rooms so early adjustments can be made.
All operations carry risk. Most patients recover without major problems, but awareness helps you respond promptly if concerns arise. Short term issues can include delayed healing along a small section of the incision, a minor collection of fluid, or localised redness. These are commonly managed with dressings, observation, and simple measures. Less frequent events include infection, bleeding, or compromised blood supply to skin or nipple tissue. Certain factors such as smoking, higher body mass index, larger resection volumes, or specific medical conditions increase the likelihood of these events. This is why the preoperative process focuses on risk reduction and optimisation.
Published studies report a range of complication rates because patient groups and techniques differ. In general, major complications are reported in a minority of cases, while temporary wound concerns are more common and typically settle with conservative care. These figures provide context rather than a prediction of any single person’s experience. Your individual risk profile is discussed during consultation so that consent is informed and tailored.
Long term considerations include the possibility of persistent sensory change, thicker scar segments in areas of higher tension, or minor asymmetry. If any of these affect comfort or function, options can be considered once healing is mature.
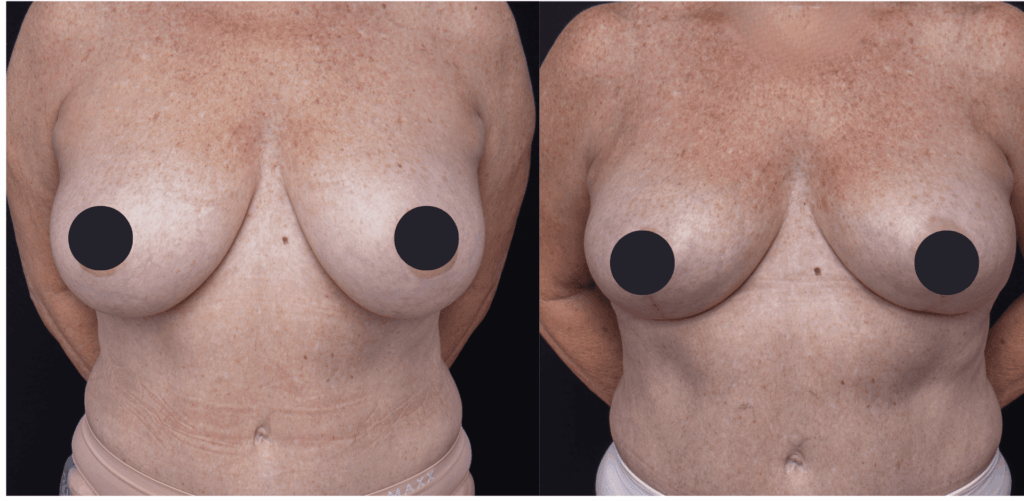
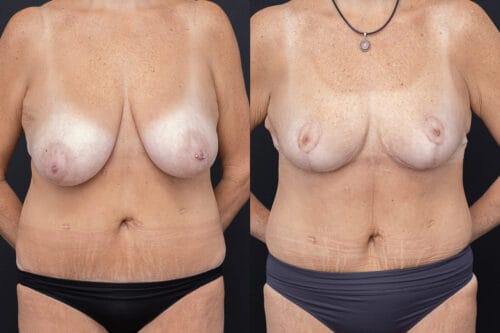
The outcomes shown are specific to those patients and may not reflect the results experienced by others, as individual outcomes can vary due to a range of factors.
Recovery is influenced by everyday choices. Aim for balanced meals that include sufficient protein, vegetables, fruit, and whole grains. Keep water intake steady. If appetite is low in the first week, have small, nutrient dense meals at regular intervals. Plan short walks to keep the circulation moving, then elevate your upper body and allow adequate sleep. Avoid smoking and keep alcohol modest, particularly while taking medication.
Wear the supportive garment as part of your treatment rather than as optional clothing. It helps control swelling, protects incisions from shear forces, and increases comfort during movement. When showering is permitted, pat the area dry and put the garment back on promptly. Avoid underwire bras until advised otherwise.
Reintroduce activity in stages. Begin with walking on level ground. Add gentle lower body exercises that do not jolt the chest. When cleared, choose lighter resistance with higher repetitions before heavier loads. Delay upper body pushing and pulling until your surgeon confirms that tissues can tolerate the demand. Monitor your response the following day and adjust accordingly.
Plan your work return honestly. Desk based roles often resume earlier than work that involves lifting, repetitive arm use, or exposure to hot and humid environments. A graded return plan can be documented at review so that duties align with your stage of healing.
Regular review supports a smooth recovery. Dr Yezdi Mistry and his Charlestown team schedule appointments that match key healing milestones. Early visits focus on wound care, garment fit, and pain control. Later visits address progression of activity, scar care, and longer term planning. If you live outside Charlestown, appointments can be arranged to balance accessibility with appropriate oversight.
Do not wait for a scheduled appointment if you are concerned. Contact the rooms if you experience increasing pain, sudden swelling on one side, spreading redness, fever, or unusual discharge from a wound. Early assessment allows straightforward problems to be managed promptly.
As healing progresses, many patients notice practical improvements that align with the reasons they sought surgery. There is often less pressure on the neck and shoulders, bra straps sit more comfortably, and exercise becomes easier to maintain. Research using validated questionnaires has documented improvements in physical wellbeing after reduction mammaplasty. While outcomes vary from person to person, planning for steady gains in comfort and function is reasonable.
Adjustment is personal. Some people feel immediate relief while others take time to recognise changes in posture, energy, and clothing choices. Maintain communication with your clinical team and keep expectations grounded in your own pace of healing.
Having your Specialist Plastic Surgeon in the local area is practical during recovery. Dr Yezdi Mistry’s rooms in Charlestown provide preoperative planning, surgery in an accredited setting, and structured follow up within the same region. This continuity makes it easier to attend reviews, ask questions, and have small concerns addressed promptly. Patients from Newcastle and the Hunter region benefit from care that is close to home and consistent.
Dr Yezdi Mistry Specialist Plastic Surgeon provides individualised guidance at each step. The approach is patient centred, with clear explanations and thoughtful planning. Recovery is approached as a partnership between patient and surgeon, with appointments used to fine tune the plan and align activities with healing.
Most swelling peaks within the first week and gradually settles over six to eight weeks. Minor residual swelling can persist for several months as tissues soften and scars mature.
Gentle walking is encouraged soon after surgery, but strenuous activity or upper body exercise should wait until cleared at review, usually around six to eight weeks postoperatively. The timeline can differ depending on your operation and healing progress.
Temporary numbness or altered sensation is common as nerves recover. Most patients regain normal or near normal sensitivity within several months, although a small number may have lasting changes.
The ability to breastfeed can vary depending on the surgical technique and the amount of tissue removed. Some women can still produce milk, but there is a risk of reduced milk supply, which is discussed before surgery.
Sleeping on your back with your upper body slightly elevated is best for the first few weeks. This position minimises swelling and pressure on healing tissues.
Not always. The decision depends on the amount of tissue removed and the surgeon’s assessment. If used, drains are typically removed within a few days once drainage is minimal.
Driving can usually resume when you can move your arms comfortably and safely control the steering wheel without pain or restriction, which for most patients is around two to three weeks.
Scars are initially pink and raised but gradually flatten and fade over 12 to 18 months. Consistent scar care, good sun protection, and adherence to aftercare instructions can help them blend with surrounding skin.
Mild asymmetry is common in the early stages as swelling rarely settles evenly. This usually improves over time, and any persistent differences can be assessed once healing is complete.
Short car trips are fine within days of surgery, but long flights or extended travel should wait until your surgeon confirms that you can sit comfortably and manage wound care. Follow up appointments are an important consideration before planning travel.
Recovery after Breast Reduction in Newcastle progresses step by step. Plan for rest in the first fortnight, expect a staged return to work and exercise over the following weeks, and allow up to a year for scars to mature and for final shape to settle. Keep in touch with your clinical team, follow the garment and wound care plan, and reintroduce activities in a measured way. These practical choices support a steady, comfortable course. If you still have questions after reading this guide, our Breast Reduction FAQs cover common concerns about recovery, sensation, scarring, and return to activity.
If you would like to discuss Recovery after Breast Reduction in Newcastle in the context of your own health and goals, or if you wish to arrange an appointment, you can contact Dr Mistry’s Charlestown clinic using the details below. This information is provided so you can reach the practice directly and book a consultation at a time that suits you.
Charlestown Healthcare Hub
Suite 312, Level 3
99 Pacific Highway
Charlestown NSW 2290
Phone: 02 4062 7888
Email: admin@drmistry.com.au
Website: www.drmistry.com.au

Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon based in Newcastle, NSW. With extensive training and experience in both reconstructive and aesthetic surgery, Dr Mistry is committed to providing safe, evidence-based care that is tailored to each patient’s individual needs.
After completing his Fellowship of the Royal Australasian College of Surgeons (FRACS) in Plastic Surgery in 2013, Dr Mistry relocated to Newcastle with his family in 2015. He began his work as a Visiting Medical Officer (VMO) in Plastic and Hand Surgery at John Hunter Hospital before establishing his private practice in 2017. His practice offers a comprehensive range of reconstructive and aesthetic procedures for the breast, body, face, and skin.
Dr Mistry’s approach to patient care is grounded in trust, respect, and open communication. From initial consultation to recovery, he aims to ensure patients feel informed, supported, and comfortable throughout their surgical journey. He is dedicated to maintaining the highest professional and ethical standards in all aspects of his work.
To remain at the forefront of modern surgical techniques, Dr Mistry continues to pursue ongoing professional development both in Australia and internationally. He was Australia’s first delegate at the Body Contouring Academy in Paris, where he received advanced training in body contouring and skin-tightening techniques, including VASER and RENUVION technologies.
Fill in your details and our friendly team will be in touch with you
Please Note: Information provided on Dr Mistry’s website is provided as a basic guide, it does not constitute a diagnosis and should not be taken as medical advice. Any surgical or invasive procedure carries risks.





“I care because it’s my job as a surgeon, as a plastic surgeon, to do the appropriate thing and to give you a good outcome. I want to leave knowing that I can tell a patient, hand on heart, that I did the very best I could and that I looked after them, so when I see them post op later that day or the next morning, that they feel they were in good hands.”
– Dr Yezdi Mistry
Request a Consult