Gynaecomastia is a condition involving the enlargement of breast tissue in males. It may appear during adolescence, early adulthood or later in life, and can involve one or both sides of the chest. Individuals often notice changes in tissue volume that persist over time and seek medical guidance to understand these developments. In Charlestown and the wider Newcastle region, many individuals consult with Dr Yezdi Mistry, Specialist Plastic and Reconstructive Surgeon, to gain clarity about their presentation and the factors that contribute to it.
Grading systems help describe gynaecomastia in a structured way. They outline how much tissue is present, whether the skin is firm or stretched, and the position of the nipple–areola complex. Grading also helps clarify whether the change is due to glandular tissue, fatty tissue, or a combination of both. These details are useful during a consultation and help guide an informed, individualised treatment plan.
This article outlines the established grading systems for gynaecomastia and explains how these systems contribute to clinical evaluation. The information follows Australian English conventions and aligns with AHPRA’s expectations for factual, balanced and responsible medical communication.
Gynaecomastia refers to the enlargement of glandular breast tissue in males. This differs from an increase in fatty tissue alone, which is known as lipomastia. Distinguishing between these two is important because glandular tissue behaves differently and may be influenced by factors such as hormonal changes, medications or systemic conditions. During a consultation with Dr Yezdi Mistry in Charlestown, examination helps clarify which components are present and whether further investigation may be helpful.
Classification provides structure to the assessment. It identifies whether the tissue increase is mild, moderate or pronounced, whether the skin has stretched in response and whether the nipple sits in a higher or lower position. Men who attend with concerns about gynaecomastia often describe noticing steady changes, long-standing enlargement from adolescence or new developments related to medications or health conditions. Grading systems allow these observations to be described in clear medical terms.
The way gynaecomastia presents varies with age. Younger individuals often have firmer glandular tissue linked to hormonal development, while older adults may have a combination of glandular and fatty tissue. Skin behaviour also changes with age, which influences how the chest appears. These differences are taken into account during an assessment at Dr Mistry’s Charlestown clinic.



The Simon classification is one of the earliest and most widely referenced systems. It places gynaecomastia into four categories based on tissue size and the presence of excess skin.
Grade I involves a small amount of tissue without excess skin. The nipple position remains typical and the chest maintains its general appearance. This is seen frequently in adolescents and may also occur in adults. During assessment, Dr Mistry evaluates the firmness of the tissue and checks whether changes appear stable.
Grade IIa describes moderate enlargement without skin excess. The increased volume is noticeable and may be visible beneath clothing. The shape of the chest changes slightly as the tissue increases. At his Charlestown practice, Dr Mistry assesses whether the enlargement is predominantly glandular or fatty, as this helps guide discussion.
Grade IIb involves moderate tissue increase with a small degree of skin stretching. The nipple may appear slightly lower compared to Grade I or IIa. Skin elasticity becomes an important factor in this grade. Individuals who have experienced weight variation or who are older may show different skin characteristics.
Grade III represents the most pronounced form within this system, involving significant tissue enlargement and visible skin redundancy. The nipple areola complex may sit lower due to the weight of the tissue. This presentation may occur in individuals with long-standing gynaecomastia or those experiencing medical or hormonal influences. Examination includes evaluation of tissue composition, skin behaviour and any contributing factors.
The Simon system provides a straightforward way to explain findings during consultation and supports informed discussion.
The Rohrich system is another classification widely referenced in clinical practice. It separates gynaecomastia into four categories that focus on tissue volume, skin redundancy and nipple position.
Grade I describes minimal enlargement without excess skin. The skin remains firm and the nipple sits in a typical position. During consultation, Dr Mistry evaluates whether the tissue is firm and localised or more diffuse.
Grade II identifies moderate enlargement with mild skin relaxation. This may develop over several years or be influenced by weight variation or hormonal activity. The change is usually more noticeable than Grade I.
Grade III features significant enlargement with moderate skin redundancy. The nipple may sit lower due to gradual stretching of the skin. Skin elasticity differs between individuals, and these variations influence assessment.
Grade IV involves marked enlargement with substantial skin redundancy and a noticeable change in nipple position. This category is often associated with long-standing changes. Dr Mistry assesses both skin and tissue characteristics when discussing clinical findings with individuals.
The Rohrich classification is useful when evaluating the behaviour of the skin and the position of the nipple in relation to the chest fold.
The Cordova and Moschella system provides a more detailed analysis by identifying tissue type, evaluating nipple position and assessing the degree of skin relaxation.
Glandular-dominant gynaecomastia presents as firm, fibrous tissue concentrated beneath the nipple area. This often occurs in adolescents, young adults or individuals affected by medications that influence hormone levels. Fatty-dominant enlargement appears softer and more diffuse and may relate more to weight variation or age. During a clinical examination, Dr Mistry palpates the tissue to determine which component is more prominent.
This classification also considers nipple position and how skin behaves as the tissue increases. These anatomical changes are helpful when assessing men who have long-standing enlargement or age-related changes.
The additional detail offered by this system supports a more comprehensive anatomical evaluation.
Gynaecomastia can occur for several reasons. Temporary hormonal fluctuations are common during adolescence, while persistent enlargement may relate to medication use, endocrine conditions, liver disease or other systemic health issues. Medications that can influence hormone levels include antiandrogens, some antidepressants, treatments for prostate conditions, certain cardiac medications and anabolic steroids.
During an appointment in Charlestown, Dr Yezdi Mistry conducts a thorough medical history that explores symptom onset, duration, past or current medications and associated health factors. Physical examination follows. This involves assessing the composition of the tissue, the elasticity of the skin, the position of the nipple and any asymmetry.
Younger individuals often present with firm glandular tissue. Older adults may have a greater proportion of fatty tissue and reduced skin elasticity. Men who have experienced weight change may have skin that behaves differently again. If there is a possibility of an underlying medical cause, further investigations such as blood tests or ultrasound may be recommended. Collaboration with general practitioners or medical specialists is common when further evaluation is appropriate.
Once the grade of gynaecomastia has been identified, the information guides clinical discussion. Grading clarifies how much tissue is present, how the skin is responding (such as whether it is firm or stretched), and the position of the nipple. This information supports an informed and individualised treatment plan.
Men with early grades and firm skin may have different considerations compared to men with more advanced grades and reduced skin elasticity. However, two individuals with the same grade may still require different approaches depending on their age, health history and anatomical variations. Grading provides structure, but the clinical process remains individualised.
Further explanation of surgical techniques is discussed in our guide to male chest reduction surgery.
Grading systems are helpful, but they cannot replace a detailed, in-person consultation. Each individual has unique anatomy influenced by age, body composition, posture, skin quality, skin tightness, or excess skin and muscle development. During appointments, Dr Yezdi Mistry explains clinical findings in clear, practical terms so individuals understand their presentation without technical complexity.
Assessment also considers factors such as shoulder position, symmetry and general chest structure. Skin quality is reviewed carefully, particularly in individuals who have experienced changes in weight. The Charlestown practice provides a professional and private environment in which individuals can discuss their concerns comfortably. Dr Mistry brings years of practising, specialist training and extensive knowledge in plastic and reconstructive surgery to every consultation.
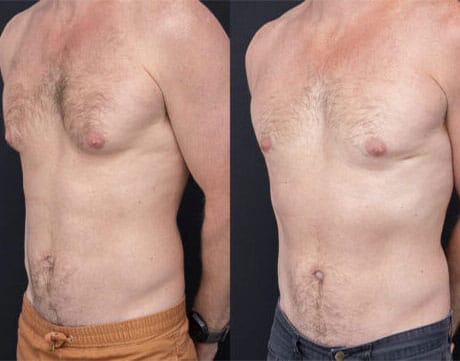
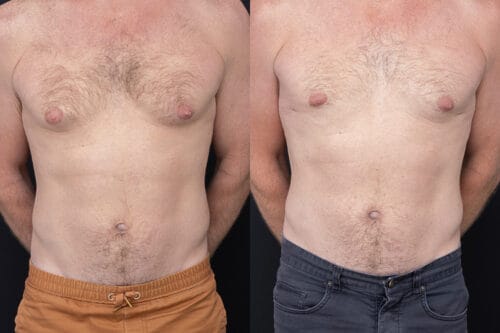
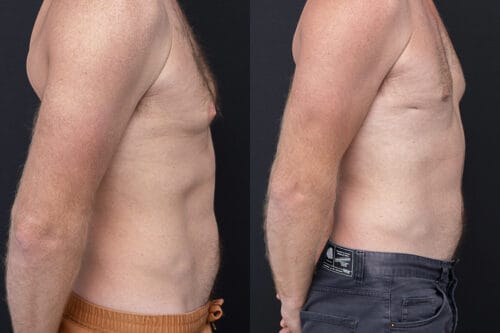
Disclaimer: The outcomes shown are specific to those patients and may not reflect the results experienced by others, as individual outcomes can vary due to a range of factors.
Gynaecomastia appears differently across age groups. Adolescents often develop firm glandular tissue during puberty. Many experience a reduction over time, although the tissue persists into adulthood for some.
Individuals in their thirties and forties often present with a mix of glandular and fatty tissue. This may relate to lifestyle factors, medications or hormonal influences. Skin may begin to show early changes in elasticity at this age.
Older adults may display more noticeable fatty tissue, reduced skin elasticity and more pronounced changes in nipple position. These age-related factors influence the grading of gynaecomastia and the clinical discussion that follows. During consultation, Dr Mistry assesses these variables to provide clear and accurate information.
Hormonal balance plays a central role in the development of gynaecomastia. An imbalance between oestrogen and androgen (reproductive hormones) activity may result in glandular tissue growth. Temporary changes during adolescence are common. Persistent imbalance may relate to medical conditions that warrant further investigation.
Some medications influence hormone levels. During consultation, Dr Mistry reviews medication history and may recommend communicating with the individual’s general practitioner if a medication may be contributing. Adjustments to medication are not made without appropriate medical coordination.
Individuals from Charlestown, Newcastle and the Hunter Region regularly visit Dr Yezdi Mistry for assessment. Access to a surgeon with specialist training and extensive clinical experience supports a thorough and informed evaluation of gynaecomastia.
During assessment, Dr Mistry reviews tissue characteristics, skin behaviour, nipple position and overall anatomy. He explains how these findings relate to recognised grading systems and what they indicate from a medical perspective. This approach supports clear communication and promotes informed decision making.
Accurate grading helps clinicians describe gynaecomastia in consistent terms. It supports structured communication and assists individuals in understanding their presentation without speculation or assumptions.
Two individuals may appear similar at first glance, yet their underlying tissue composition and skin behaviour may differ considerably. Grading identifies these distinctions and helps guide discussion during consultation.
Using established systems such as Simon, Rohrich and Cordova and Moschella allows Dr Mistry to provide a detailed yet clear explanation during appointments. This supports individuals as they explore their options and understand their condition in medically accurate terms.
Yes, the grade may change depending on factors such as age, hormonal variation or weight changes. Some individuals notice that the tissue becomes firmer or softer over time, and the nipple position may also shift. A clinical assessment helps clarify these developments.
Asymmetry is common, and each side may present with a different amount of tissue or skin behaviour. These differences are evaluated individually during consultation because each side may require a tailored clinical approach.
The grade alone does not determine the need for investigations. Tests are recommended based on medical history, timing of onset and any relevant symptoms. Blood tests or imaging may be suggested if clinically appropriate.
Certain medications can contribute to the development or progression of gynaecomastia. If medication is suspected as a contributing factor, this is reviewed carefully and may involve collaboration with the individual’s general practitioner. Any change to medication requires appropriate medical coordination.
Body weight can influence the amount of fatty tissue in the chest but does not necessarily reflect the glandular component. Physical examination is important to differentiate between the two. Both aspects are assessed during consultation.
Hormonal variation, particularly during adolescence, may cause temporary increases in glandular tissue. These changes can stabilise over time, but persistent enlargement may warrant further assessment. Hormonal factors are considered during evaluation with Dr Mistry.
Changes in nipple sensitivity may occur in some individuals, but this varies widely. Sensitivity does not reliably indicate the grade and is reviewed separately during consultation.
Exercise may alter fatty tissue in the chest but does not modify glandular tissue. Strength training may change the appearance of the chest muscles, but it does not adjust the underlying glandular component. This distinction is explained clearly during assessment.
Higher grades often involve changes in skin quality and tightness, but this depends on age, genetics and weight variation. Skin response varies between individuals and is evaluated during physical examination.
Tenderness may occur in any grade, especially in cases influenced by hormonal activity. It does not define the grade but provides additional context during assessment. Dr Mistry considers this along with other clinical findings.
Men who wish to understand their chest changes can arrange a consultation with Dr Yezdi Mistry at his Charlestown practice. The appointment process involves a thorough assessment and clear explanation of clinical findings. Dr Mistry’s specialist training, clinical experience and years of practising contribute to detailed and responsible evaluation. Discussions remain aligned with AHPRA standards and focus on providing accurate, balanced medical information.

Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon based in Newcastle, NSW. With extensive training and experience in both reconstructive and aesthetic surgery, Dr Mistry is committed to providing safe, evidence-based care that is tailored to each patient’s individual needs.
After completing his Fellowship of the Royal Australasian College of Surgeons (FRACS) in Plastic Surgery in 2013, Dr Mistry relocated to Newcastle with his family in 2015. He began his work as a Visiting Medical Officer (VMO) in Plastic and Hand Surgery at John Hunter Hospital before establishing his private practice in 2017. His practice offers a comprehensive range of reconstructive and aesthetic procedures for the breast, body, face, and skin.
Dr Mistry’s approach to patient care is grounded in trust, respect, and open communication. From initial consultation to recovery, he aims to ensure patients feel informed, supported, and comfortable throughout their surgical journey. He is dedicated to maintaining the highest professional and ethical standards in all aspects of his work.
To remain at the forefront of modern surgical techniques, Dr Mistry continues to pursue ongoing professional development both in Australia and internationally. He was Australia’s first delegate at the Body Contouring Academy in Paris, where he received advanced training in body contouring and skin-tightening techniques, including VASER and RENUVION technologies.
Professional Memberships:
Fill in your details and our friendly team will be in touch with you
Please Note: Information provided on Dr Mistry’s website is provided as a basic guide, it does not constitute a diagnosis and should not be taken as medical advice. Any surgical or invasive procedure carries risks.





“I care because it’s my job as a surgeon, as a plastic surgeon, to do the appropriate thing and to give you a good outcome. I want to leave knowing that I can tell a patient, hand on heart, that I did the very best I could and that I looked after them, so when I see them post op later that day or the next morning, that they feel they were in good hands.”
– Dr Yezdi Mistry
Request a Consult