Adult gynaecomastia refers to the development of glandular breast tissue in males. It is a relatively common condition that can appear at different stages of life, and although it is usually benign, individuals often seek information to understand why it has developed and whether any assessment is appropriate.
Some men notice firmness behind the nipple, others observe gradual changes in the chest, and some experience temporary tenderness. Because the causes are varied, a structured approach to evaluation is important.
Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon in Newcastle NSW and regularly performs Gynecomastia surgery.
Gynaecomastia involves an increase in glandular breast tissue in males. This tissue typically forms beneath the nipple and areola and may feel firmer than the surrounding chest fat. It is distinct from chest fullness related primarily to adipose tissue. True gynaecomastia is influenced by hormonal factors, particularly when the balance between androgens and oestrogen changes.
Men naturally produce both androgens and oestrogen. Testosterone usually plays the dominant role in male breast tissue, but when this balance shifts, glandular tissue may develop. This does not automatically indicate a medical problem. Hormonal changes occur at many points in life, including adolescence, early adulthood and older age. Some individuals develop small stable areas of glandular tissue that never change, while others notice gradual development over time.
Because gynaecomastia can resemble other conditions and may sometimes overlap with systemic or endocrine issues, a clinical evaluation offers clarity and allows appropriate management planning.


Gynaecomastia is more common than many people expect. Studies show that a large proportion of males experience some degree of glandular breast tissue growth during puberty. While many cases reduce as hormones stabilise, some persist into adulthood.
Adult gynaecomastia is also seen in men in their twenties, thirties, forties and older. Age related hormonal change, variations in body composition, medication use and other health conditions can all contribute. The condition may affect one or both sides of the chest, and asymmetry is frequent. This does not necessarily indicate a concerning cause, but asymmetry is one of the reasons an assessment may be recommended.
Because the condition is common, the significance lies not in its presence alone but in understanding its cause and how it behaves over time.
Gynaecomastia can develop for many reasons. In some cases, one clear factor is present. In others, several influences combine.
Age related hormonal change is a common contributor. Testosterone levels can decrease gradually as men age. Changes in body composition may also play a role because fat tissue contains enzymes that convert androgens to oestrogen. This process may influence the hormonal environment and contribute to glandular development.
Medication related gynaecomastia is well recognised. Medicines prescribed for prostate conditions, some cardiac medications, spironolactone, certain antidepressants, antipsychotics, anti ulcer treatments and HIV medications may influence hormone activity or metabolism. A medication review during assessment can provide important insights.
The use of anabolic agents for muscle building can disrupt the natural hormonal feedback system. This may increase the conversion of hormones to oestrogen or reduce natural testosterone production. Alcohol, cannabis and other recreational drugs may also influence hormone levels or liver metabolism.
Endocrine and systemic conditions represent another group of potential causes. Thyroid overactivity, testicular conditions, tumours influencing hormone production, chronic liver disease and chronic kidney disease may each contribute in different ways. These conditions vary in severity, and identifying them ensures appropriate management.
Genetic and chromosomal conditions, such as Klinefelter syndrome, are less common but relevant. They influence hormonal development and may increase the likelihood of gynaecomastia.
In many cases, no clear cause is identified. This is known as idiopathic gynaecomastia. Even when the cause is not found, an assessment helps rule out concerning health issues and assists individuals in understanding appropriate management options.
The presentation varies widely. Some men notice a firm, circular area beneath the nipple. Others observe a broader change across the chest. Tenderness can occur, particularly when glandular tissue is developing. This may be noticed during physical activities, pressure or friction from clothing.
Asymmetry is common. One side may appear more developed than the other. While this often reflects normal variation, unilateral changes are assessed carefully because male breast cancer usually presents on one side. Although male breast cancer is rare, distinguishing between benign and concerning features is a central part of evaluation.
Certain signs require prompt review. These include irregular lumps not centred beneath the nipple, skin changes, nipple discharge, nipple inversion or swelling in the armpit. These features may be unrelated to cancer but should always be assessed.
Diagnosis involves a structured clinical assessment. Dr Yezdi Mistry, a Specialist Plastic and Reconstructive Surgeon in Newcastle with extensive knowledge and clinical experience, begins with a detailed medical history and examination.
The history includes the onset of changes, progression over time, any associated sensitivity and a full review of medications, supplements and substances. Many individuals are unaware that some medications influence hormone levels, so this discussion is important. A review of overall health, endocrine symptoms and previous medical conditions may provide further insight.
The physical examination assesses the breast tissue, nipple and surrounding structures. The distribution of glandular tissue, firmness, sensitivity and asymmetry are evaluated. Examination of the testicles and assessment for signs of systemic disease may also form part of the evaluation.
Blood tests may be recommended to assess hormone levels and organ function. These can include testosterone, oestradiol, luteinising hormone, follicle-stimulating hormone, thyroid tests, liver tests, kidney tests and, where appropriate, human chorionic gonadotropin. Testing is tailored to the individual rather than performed in every case.
Imaging may be indicated in certain circumstances. Ultrasound assists in characterising tissue and identifying unusual features. Mammography may be used when required. Testicular ultrasound may be recommended if there are concerns about hormone-producing conditions.
This structured approach ensures that the diagnosis is accurate and that management decisions are based on current evidence and individual factors.

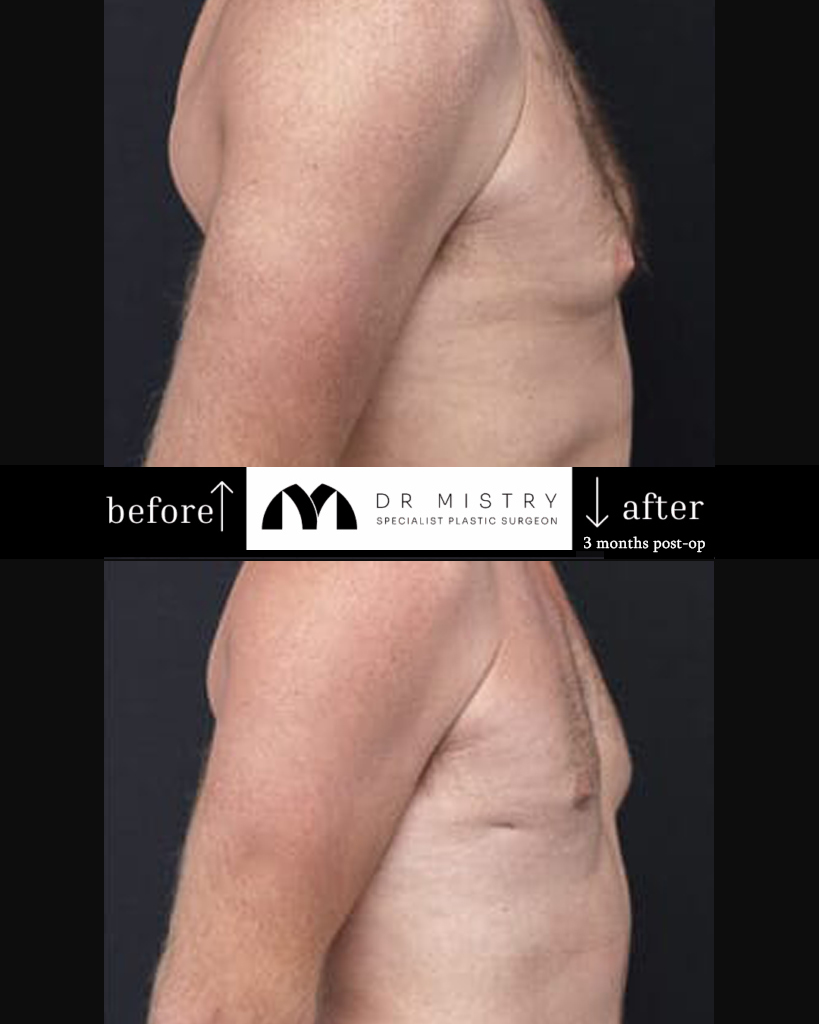
Management depends on the cause, the duration of the condition, the extent of glandular development and the individual’s goals. Many individuals do not require treatment beyond reassurance and monitoring.
Observation is suitable when gynaecomastia is mild, stable or related to temporary hormonal changes. If medication-related causes are identified, the prescribing doctor may adjust treatment if medically appropriate.
Medical therapy may be considered for individuals experiencing tenderness, particularly when the condition is relatively new. Medications that influence oestrogen receptors may support symptom reduction in some cases, but their use requires specialist oversight and is not suitable for everyone.
Surgical treatment may be discussed for long-standing gynaecomastia that contains firm glandular tissue. Surgery aims to remove glandular tissue and, when appropriate, address associated fat. Some men have both components, and the surgical plan may incorporate different techniques to address them.
At his Newcastle practice, Dr Mistry provides an individualised assessment that considers tissue characteristics, anatomy and personal goals. Technologies such as VASER may be used in selected cases to address fat, depending on suitability. Surgical treatment is planned carefully, and individuals receive clear information about expected outcomes and limitations.
All surgical procedures carry risks. These include bleeding, infection, changes in nipple sensation, asymmetry, changes in chest shape, delayed healing, fluid accumulation and scarring. Serious complications such as blood clots are uncommon but possible. During consultation, Dr Mistry outlines these risks clearly and explains strategies to support risk reduction.
Surgery addresses existing glandular tissue but does not prevent further development if contributing factors persist. Continued medication use, anabolic agent use or unmanaged endocrine conditions may influence future changes. Weight variation may also affect chest appearance over time.
Understanding these considerations supports realistic expectations and informed decision-making.
Recovery varies. Individuals commonly experience swelling, bruising and temporary discomfort during the early phase. Compression garments may be recommended to support the chest and assist with swelling. Light activities may be resumed early, while strenuous exercise and heavy lifting are usually delayed for several weeks.
Healing continues over several months. Follow up appointments allow Dr Mistry to monitor progress, assess healing and offer personalised guidance. His focused practice in plastic and reconstructive surgery supports a steady and well managed recovery process.
Some individuals notice periods where the glandular tissue feels more prominent due to hormonal variation, weight change or temporary inflammation. These fluctuations usually stabilise, but ongoing changes may prompt a clinical assessment to clarify contributing factors.
Yes, some men have small areas of glandular tissue that are only noticeable on examination. These cases may remain stable for years and often come to attention only during a medical review for other reasons.
Exercise can strengthen the underlying muscles, but it does not remove glandular tissue if it is present. In some cases, increased muscle bulk may make the glandular tissue more noticeable, which is why assessment can help identify the underlying components.
Some people describe temporary sensitivity or firmness related to activity, temperature or hormonal fluctuations. These patterns are usually benign, although persistent changes may warrant review.
Long-standing tissue may become firmer due to natural changes in the gland over time. Newer cases may feel more sensitive or tender, and management options may differ depending on duration.
Yes, many individuals diagnosed with gynaecomastia have hormone levels within normal ranges. The condition can occur due to local tissue sensitivity or subtle variations not captured in routine testing.
Glandular tissue often begins beneath the nipple and may remain localised to this region. This can make the area feel firmer even when the surrounding chest appears unchanged.
Some supplements contain ingredients that may influence hormone levels or metabolism. Discussing all supplements during your assessment helps determine whether they may be contributing factors.
Weight variation can change the appearance of the chest due to changes in fat distribution. While glandular tissue itself does not resolve with weight loss, an assessment can help determine the proportion of glandular and fat-related components.
Yes, many men with gynaecomastia experience no discomfort. The absence of tenderness does not exclude glandular tissue, which is why clinical assessment focuses on examination rather than symptoms alone.
For many men, gynaecomastia does not require active treatment. Some choose monitoring, while others may explore treatment after considering their circumstances. The most appropriate approach depends on the cause, symptoms and personal preferences.
A structured evaluation provides clarity. Whether the recommended pathway involves observation, medical management or surgery, the goal is to provide accurate information in a balanced and accessible way.
Because gynaecomastia can have many contributing factors, assessment by a specialist with extensive training is important. Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon based at Suite 312, Level 3, Charlestown Healthcare Hub, 99 Pacific Highway. His long-standing professional background, detailed understanding of male chest anatomy and continued national and international training support high standards of clinical care.
Individuals in Newcastle and the Hunter region often seek his guidance to understand the cause of their gynaecomastia and explore management options. Dr Mistry provides individualised advice, discusses non-surgical and surgical pathways and supports decision-making based on accurate information.
Adults in Newcastle or the Hunter region seeking assessment for gynaecomastia can arrange a consultation with Dr Yezdi Mistry at the Charlestown Healthcare Hub. During the consultation, Dr Mistry conducts a detailed evaluation, reviews medical history and discusses potential management pathways.

Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon based in Newcastle, NSW. With extensive training and experience in both reconstructive and aesthetic surgery, Dr Mistry is committed to providing safe, evidence-based care that is tailored to each patient’s individual needs.
After completing his Fellowship of the Royal Australasian College of Surgeons (FRACS) in Plastic Surgery in 2013, Dr Mistry relocated to Newcastle with his family in 2015. He began his work as a Visiting Medical Officer (VMO) in Plastic and Hand Surgery at John Hunter Hospital before establishing his private practice in 2017. His practice offers a comprehensive range of reconstructive and aesthetic procedures for the breast, body, face, and skin.
Dr Mistry’s approach to patient care is grounded in trust, respect, and open communication. From initial consultation to recovery, he aims to ensure patients feel informed, supported, and comfortable throughout their surgical journey. He is dedicated to maintaining the highest professional and ethical standards in all aspects of his work.
To remain at the forefront of modern surgical techniques, Dr Mistry continues to pursue ongoing professional development both in Australia and internationally. He was Australia’s first delegate at the Body Contouring Academy in Paris, where he received advanced training in body contouring and skin-tightening techniques, including VASER and RENUVION technologies.
Professional Memberships:
Fill in your details and our friendly team will be in touch with you
Please Note: Information provided on Dr Mistry’s website is provided as a basic guide, it does not constitute a diagnosis and should not be taken as medical advice. Any surgical or invasive procedure carries risks.





“I care because it’s my job as a surgeon, as a plastic surgeon, to do the appropriate thing and to give you a good outcome. I want to leave knowing that I can tell a patient, hand on heart, that I did the very best I could and that I looked after them, so when I see them post op later that day or the next morning, that they feel they were in good hands.”
– Dr Yezdi Mistry
Request a Consult