Gynaecomastia surgery is a procedure performed by Dr Yezdi Mistry, Specialist Plastic and Reconstructive Surgeon (BHB, MBChB, FRACS Plastic Surgery), based in Charlestown, NSW. The surgery is designed for men with persistent enlargement of breast tissue that has not improved with observation, lifestyle changes or medical review. Depending on the underlying cause, the procedure may involve removal of firm glandular tissue, targeted removal of fatty tissue using specialised liposuction techniques, or a combination of both approaches. Dr Mistry assesses the proportion of glandular versus fatty tissue, skin quality and the overall chest anatomy to determine which technique or combination of techniques is most appropriate.
Gynaecomastia surgery is performed in accredited hospital facilities under general anaesthesia. Incisions are planned carefully, often placed around the areola or within discreet areas of the chest, depending on the surgical needs identified during consultation. A compression garment is worn after surgery to support the chest as swelling settles, and follow-up appointments are scheduled to review healing and progress over time. Dr Mistry provides clear explanations about each operative step so that patients understand what the procedure can address and what factors may influence the final outcome.
Men who have persistent enlargement of the breast area that has not improved with time, lifestyle measures or medical assessment may be considered for surgery. Suitability requires a thorough evaluation with Dr Mistry, who reviews medical history and contributing factors. The aim is to determine whether surgery is appropriate and whether another underlying cause requires attention first.
Most individuals are adults, as breast tissue changes during puberty often settle on their own. Younger patients may be considered only after stability of breast tissue has been confirmed. Dr Mistry ensures the timing is clinically appropriate before recommending any operative approach.
During consultation, Dr Mistry performs a clinical examination to distinguish between glandular tissue, fatty tissue or a combination. In some cases, imaging may help clarify the underlying cause. This assessment guides the surgical approach used.
Learn about Adult Gynaecomastia.
Hormonal variations can contribute to breast tissue enlargement, and these factors are explored during consultation. If a hormonal imbalance is suspected, appropriate investigations may be recommended. Surgery is considered only once underlying causes have been reviewed.
Weight can influence the appearance of the chest area, and in some cases weight stabilisation may be recommended before surgery. Dr Mistry discusses how weight and body composition relate to the result. This helps set clear expectations for what surgery may achieve.
Certain medications may contribute to tissue enlargement. If this is suspected, the prescribing doctor may consider alternatives before surgery is planned. Dr Mistry reviews all relevant history to ensure the timing and suitability of surgery are appropriate.
Exercise may improve overall chest tone but cannot remove glandular tissue. If glandular enlargement is the primary concern, surgery may be the only effective option. Dr Mistry discusses non-operative and operative pathways during consultation.
Read: Everything You Need To Know About Male Chest Reduction Surgery.
If enlargement persists beyond several months despite lifestyle measures or medical review, surgery may be discussed. Pubertal changes often resolve naturally, so waiting until tissue stability is confirmed is recommended. Dr Mistry assesses duration and progression during the consultation.
Certain conditions may influence healing or surgical planning. These are reviewed carefully so that any health considerations are addressed beforehand. This ensures the procedure is planned with an emphasis on medical appropriateness.
Smoking affects wound healing and may compromise the quality of the result. Dr Mistry will request smoking cessation before surgery and discuss timelines appropriate for each patient. This supports safer recovery.
Dr Mistry conducts a detailed medical assessment, examines the chest and discusses treatment goals. Imaging or further tests may be recommended if needed. This consultation helps establish a personalised plan suited to the patient’s clinical profile.
Routine blood tests or imaging may be needed depending on medical history. These assessments help ensure suitability and identify any factors that may influence the procedure. Dr Mistry reviews results before confirming readiness for surgery.
Some medications or supplements may need to be paused temporarily. Dr Mistry provides individualised instructions to maintain safety. Clear guidance is supplied in writing to support preparation.
Regular physical activity is generally encouraged, but strenuous training may need to be modified close to the procedure. Dr Mistry explains appropriate timelines for activity adjustments. This helps facilitate smoother planning and recovery.
Maintaining stable weight, good nutrition and healthy habits supports healing. Adequate hydration and sleep may also be beneficial. Dr Mistry provides tailored advice where appropriate.
Fasting instructions are standard for procedures involving anaesthesia. Patients receive specific timing requirements from the hospital and Dr Mistry’s team. Following these instructions is important for safety on the day.
A support person is recommended to assist with transport and early post-operative care. This ensures patients return home comfortably and follow immediate post-operative instructions. Written guidance is provided before the day.
Loose, front-opening garments are usually most comfortable after chest procedures. This allows easier movement and reduces strain on the area. Dr Mistry’s team provides recommendations ahead of time.
Some supplements may influence bleeding or healing. Dr Mistry reviews all products taken and advises which should be paused. This cautious approach supports a safer operative plan.
Alcohol may affect healing and anaesthesia. Reducing or avoiding alcohol in the lead-up to surgery is generally advised. Dr Mistry outlines appropriate timelines for each patient.
All surgical procedures carry potential risks, including bleeding, infection or changes in sensation. Dr Mistry discusses these in detail so that patients can make informed decisions. Each individual’s risk profile is assessed during consultation.
Recurrence is uncommon but may occur if contributing factors, such as certain medications or significant weight changes, arise. Dr Mistry discusses factors that may influence long-term stability. A personalised approach helps set realistic expectations.
Temporary changes may occur as nerves recover after surgery. In some cases, sensation differences may persist. Dr Mistry explains possible outcomes and what to expect during healing.
Incision placement is planned to minimise visibility where possible. Visibility varies depending on skin type, healing characteristics and the surgical technique used. Dr Mistry provides individualised guidance based on examination.
Some natural asymmetry exists in most individuals, and residual differences may remain. Dr Mistry takes care to address asymmetry where possible within anatomical limits. These considerations are reviewed during planning.
Swelling, firmness or temporary contour irregularities may occur as tissues settle. These changes gradually improve over time. Follow-up appointments allow Dr Mistry to monitor progress.
Predictability depends on factors such as tissue characteristics and healing responses. Dr Mistry provides clear information on anticipated changes based on clinical examination. This supports informed decision-making.
In some circumstances, additional refinement may be considered after tissues have fully healed. This is discussed on a case-by-case basis. Dr Mistry explains when and why revision may be appropriate.
Post-operative scar care can support optimal healing. Dr Mistry provides evidence-based guidance tailored to each patient’s skin type. Consistent care may help refine the appearance over time.
Follow-up helps monitor healing and long-term tissue stability. Dr Mistry recommends appointments based on individual needs. This ensures ongoing clinical support.
Surgery may involve glandular tissue removal, liposuction techniques or a combination of both. The specific approach depends on the proportion of fatty and glandular tissue present. Dr Mistry explains the planned method during consultation.
This procedure is usually performed under general anaesthesia. An experienced anaesthetist monitors patients throughout. Dr Mistry collaborates closely with the anaesthetic team to support safety.
Timing varies depending on the amount of tissue involved and the technique used. Dr Mistry provides approximate timelines during consultation. Efficiency is balanced with meticulous planning and execution.
In some cases, small drains may be placed to manage early post-operative fluid. Their use depends on tissue characteristics and the surgical approach. Patients are given clear instructions on care if drains are required.
Incisions are usually positioned around the edge of the areola or in discreet areas of the chest. Placement is planned according to tissue needs and access requirements. Dr Mistry explains the rationale behind each approach.
Liposuction may be used when fatty tissue contributes significantly to chest fullness. If glandular tissue predominates, excision alone may be appropriate. Dr Mistry determines this during examination.
Careful technique and specialised equipment help control bleeding. This is an important part of producing a safe operative environment. The anaesthetic team also assists in monitoring throughout.
A compression garment is applied to assist with swelling and support. This is worn for a period determined by Dr Mistry. Detailed instructions are provided for correct use.
Many patients return home the same day, although some circumstances may require a short stay. This depends on individual health factors and the procedure performed. Dr Mistry discusses what is appropriate for each patient.
Patients are monitored in recovery until they are stable and comfortable. Pain management and initial care instructions are reviewed. Dr Mistry’s team ensures patients understand early post-operative requirements before discharge.
Swelling, firmness and discomfort are common early experiences. These symptoms gradually improve as healing progresses. Dr Mistry provides tailored instructions to support safe recovery.
Light activities can usually be resumed relatively soon, while more strenuous tasks require additional time. Dr Mistry outlines activity schedules appropriate for the individual and the technique used. Returning to exercise is guided carefully.
The garment helps manage swelling and supports tissue settling. Dr Mistry provides specific guidance on duration and fit. Consistent use is an important part of early recovery.
Follow-up visits occur at set intervals to monitor progress and address questions. These appointments allow Dr Mistry to assess healing and adjust care as needed. Patients are encouraged to attend all recommended reviews.
Any unexpected redness, worsening pain, excessive swelling or discharge should be reported promptly. Early communication allows timely assessment. Dr Mistry’s team provides clear information on what to monitor.
Swelling gradually reduces over weeks, with more subtle changes continuing for several months. Tissue softening occurs progressively. Dr Mistry explains typical timelines during consultation.
Most individuals return to desk-based duties relatively soon, while physical roles may require longer. Timing depends on the extent of surgery and occupational demands. Guidance is personalised.
In some cases, gentle massage techniques may be advised once healing has progressed. Dr Mistry provides instructions only when appropriate for the individual. These techniques are not introduced until tissues are ready.
Gradual reintroduction of exercise is recommended, with avoidance of heavy upper-body training initially. Dr Mistry outlines a staged plan tailored to each patient. This approach supports predictable healing.
Changes in sensation, firmness and tightness improve over time. Most individuals notice progressive settling over several months. Dr Mistry reviews progress at each follow-up.
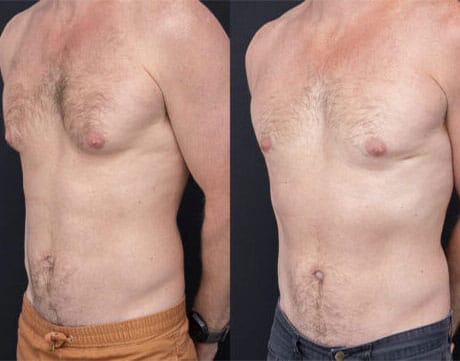
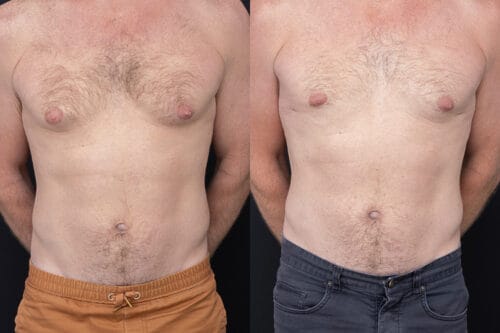
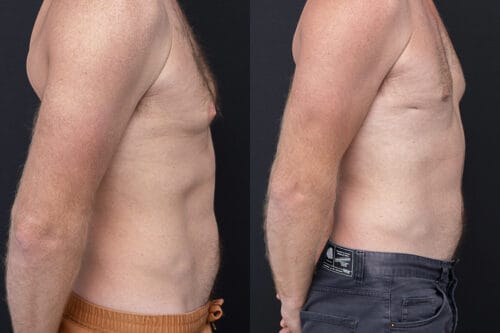
Disclaimer: The outcomes shown are specific to those patients and may not reflect the results experienced by others, as individual outcomes can vary due to a range of factors.
Gynaecomastia surgery is designed to address persistent enlargement of breast tissue in men when appropriate medical or lifestyle measures have not led to improvement. The procedure is tailored to the individual, as some men experience excess glandular tissue, others have fatty tissue contributing to chest prominence, and many present with a combination. This difference influences whether excision, liposuction or a combined approach is used. During consultation, Dr Yezdi Mistry evaluates the tissue characteristics, skin quality, medical history and contributing factors to determine the most suitable surgical plan.
The aim of surgery is to create a flatter, more proportional chest contour while adhering to safe operative principles and evidence-based practice. Incisions are planned carefully to minimise visibility, and operative steps are explained in detail to ensure that each patient understands what to expect.
Healing occurs gradually, and Dr Mistry emphasises the importance of structured follow-up care to monitor progress, support recovery and address any questions that arise. By combining clinical assessment, surgical precision and ongoing review, Dr Mistry provides a clear and informed pathway for individuals considering this procedure.
Men experiencing persistent breast tissue enlargement and seeking further information are encouraged to arrange a consultation with Dr Yezdi Mistry at his Charlestown practice. This appointment provides an opportunity to discuss the history of the condition, previous treatments, contributing factors and any concerns or goals the patient may have. Dr Mistry undertakes a detailed examination to determine whether surgery is appropriate and explains the operative plan, recovery expectations and potential risks in clear, practical terms. This ensures that each individual has the information needed to make a well-informed decision.
The consultation also allows patients to understand how preparation, post-operative care and follow-up will be structured should they choose to proceed. Dr Mistry and his team guide patients through each stage of the process, offering support from the initial enquiry through to long-term review. Those wishing to explore whether treatment may be suitable for their circumstances are welcome to contact the Charlestown clinic to begin the process.

Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon based in Newcastle, NSW. With extensive training and experience in both reconstructive and aesthetic surgery, Dr Mistry is committed to providing safe, evidence-based care that is tailored to each patient’s individual needs.
After completing his Fellowship of the Royal Australasian College of Surgeons (FRACS) in Plastic Surgery in 2013, Dr Mistry relocated to Newcastle with his family in 2015. He began his work as a Visiting Medical Officer (VMO) in Plastic and Hand Surgery at John Hunter Hospital before establishing his private practice in 2017. His practice offers a comprehensive range of reconstructive and aesthetic procedures for the breast, body, face, and skin.
Dr Mistry’s approach to patient care is grounded in trust, respect, and open communication. From initial consultation to recovery, he aims to ensure patients feel informed, supported, and comfortable throughout their surgical journey. He is dedicated to maintaining the highest professional and ethical standards in all aspects of his work.
To remain at the forefront of modern surgical techniques, Dr Mistry continues to pursue ongoing professional development both in Australia and internationally. He was Australia’s first delegate at the Body Contouring Academy in Paris, where he received advanced training in body contouring and skin-tightening techniques, including VASER and RENUVION technologies.
Professional Memberships:
Fill in your details and our friendly team will be in touch with you
Please Note: Information provided on Dr Mistry’s website is provided as a basic guide, it does not constitute a diagnosis and should not be taken as medical advice. Any surgical or invasive procedure carries risks.





“I care because it’s my job as a surgeon, as a plastic surgeon, to do the appropriate thing and to give you a good outcome. I want to leave knowing that I can tell a patient, hand on heart, that I did the very best I could and that I looked after them, so when I see them post op later that day or the next morning, that they feel they were in good hands.”
– Dr Yezdi Mistry
Request a Consult