Men often seek clear information about changes they have observed in the chest area, and two commonly discussed patterns are true gynaecomastia and pseudogynaecomastia. Although these conditions may look similar, they arise from different types of tissue, so understanding how they differ can help guide informed discussions during a medical assessment. Many individuals are unsure whether the changes they notice relate to glandular tissue, adipose tissue or a combination of both, which is why a detailed explanation of each pattern can be helpful before attending a consultation.
Dr Yezdi Mistry, Specialist Plastic and Reconstructive Surgeon in Charlestown, NSW, has extensive clinical experience assessing male chest conditions as part of his focused practice. His background includes FRACS accreditation, years of practising across both public and private settings and ongoing involvement in national and international training programs. This article outlines key information about true gynaecomastia and pseudogynaecomastia, drawing on peer reviewed evidence and reflecting Dr Mistry’s patient centred communication style. It is designed to support individuals in Newcastle who are seeking clear, reliable and medically grounded information before discussing their own circumstances in detail.
True gynaecomastia involves an increase in glandular breast tissue in males. This tissue is structured and hormonally responsive. When it increases, individuals may notice a firm area beneath or around the nipple areolar complex. Some experience local tenderness, particularly if the change has occurred recently.
This process is influenced by the balance between oestrogen and androgen activity. Both hormones are naturally present in males, but a relative increase in oestrogen activity can contribute to glandular tissue development. This type of chest change is benign but may prompt individuals to seek further information or clinical assessment.
True gynaecomastia is seen in newborns, adolescents and older men. In many cases it stabilises without intervention. When it persists or progresses, further evaluation may identify contributing factors such as medication use or underlying medical conditions.


Pseudogynaecomastia refers to fullness in the chest that is primarily related to adipose tissue rather than glandular breast tissue. The area generally feels softer and more diffuse. Some individuals notice that this pattern changes with body weight because adipose tissue responds to weight fluctuations.
Pseudogynaecomastia is common in men with increased body mass or central adiposity (carrying extra fat around the abdomen/belly area). Genetic and lifestyle factors may influence how and where adipose tissue is distributed. In some cases, pseudogynaecomastia occurs alongside true gynaecomastia, resulting in both adipose and glandular elements.
Although true gynaecomastia and pseudogynaecomastia can appear similar, the difference in tissue type influences the assessment and the discussions that follow. Some individuals aim to address these changes through weight management, which may alter adipose tissue but not glandular tissue. Others may assume surgical treatment is the only available option when a medical review or lifestyle adjustments may be appropriate.
Determining whether glandular tissue, adipose tissue or a combined pattern is present allows clinicians to guide suitable next steps. True gynaecomastia may relate to hormonal, medical or medication associated factors, while pseudogynaecomastia often relates to adipose distribution.
Dr Mistry uses a structured assessment that includes a detailed history, examination and, when suitable, further investigations.
Hormonal balance plays a central role in true gynaecomastia. A relative increase in oestrogen activity or a decrease in androgen activity may contribute to the development of glandular breast tissue.
Several situations are recognised. Physiological gynaecomastia occurs in newborns, adolescents and older men. Outside these stages, other contributors may be involved. Certain medications such as some cardiovascular drugs, antiandrogens, antidepressants, antiulcer medications and specific antiretroviral therapies have been linked to gynaecomastia. Substances including anabolic steroids, alcohol and some recreational drugs can also influence hormone activity.
Medical conditions affecting the thyroid, liver or kidneys may play a role because these organs are involved in hormone processing. Testicular conditions may also contribute.
A structured medical evaluation helps identify relevant factors, particularly when changes develop outside expected physiological windows.
Pseudogynaecomastia results from adipose tissue accumulation. Weight gain is the most common contributor, although genetic factors can influence distribution. You can read more about this in Does Being Overweight Cause Gynaecomastia? Causes, Signs and Effects. Adipose tissue itself participates in hormonal processes, and individuals with higher levels of adiposity may also present with mixed patterns involving both adipose and glandular components.
Individuals who reduce body weight may notice changes in the adipose portion of chest fullness. Glandular tissue, however, does not typically respond to weight changes in the same way.
During examination, Dr Mistry evaluates tissue quality, firmness and distribution. True gynaecomastia is often associated with a firm, structured area beneath the nipple areolar complex. This tissue may be sensitive in early stages.
Pseudogynaecomastia typically feels soft and diffuse. The tissue often shifts in a manner that aligns with adipose characteristics when individuals change position.
Asymmetry may occur in both patterns. If clinical findings suggest the need for further clarity, imaging may assist in understanding the tissue components present.
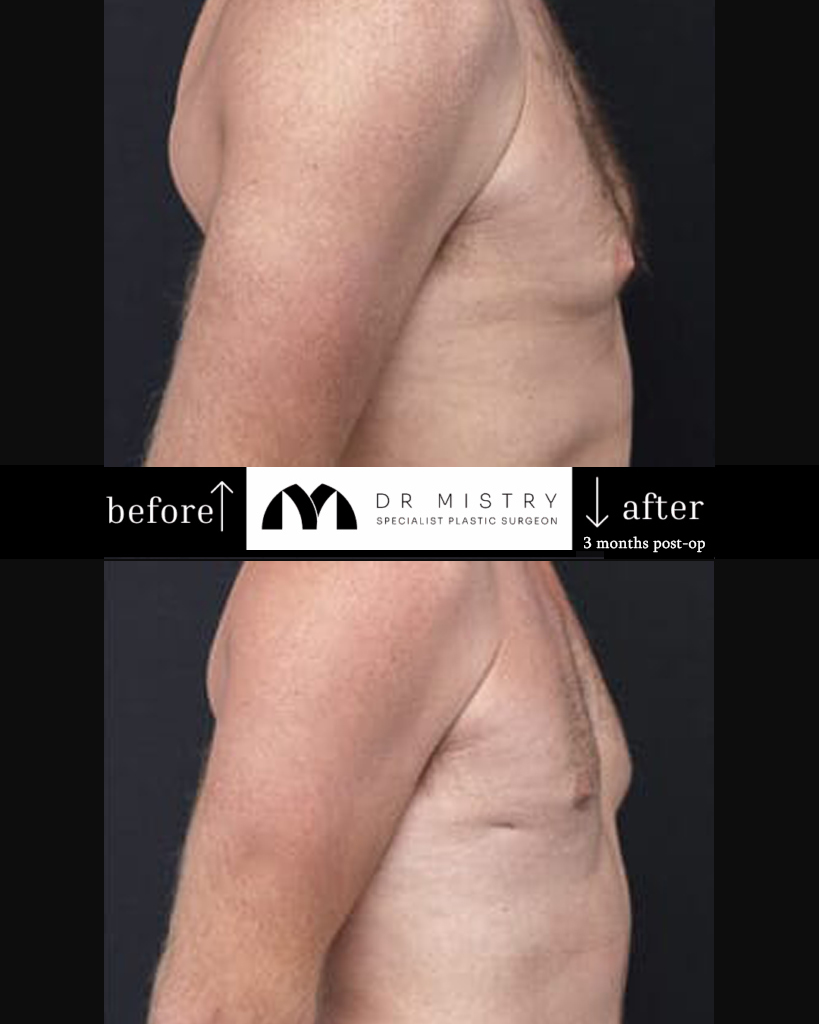
Disclaimer: The outcomes shown are specific to those patients and may not reflect the results experienced by others, as individual outcomes can vary due to a range of factors.


Assessment begins with a detailed discussion of medical history. Individuals are asked about the timing and progression of changes, any related symptoms and all medications or supplements used. This helps identify factors that may contribute to hormonal variation or tissue changes.
A structured physical examination follows. This includes assessing the chest, testicular examination and a general health review. If suitable, laboratory tests may be requested, including hormone studies and assessments of liver, kidney and thyroid function.
Imaging may be recommended to distinguish between tissue types or to investigate findings that require additional clarification. Ultrasound is commonly used for this purpose.
Not all presentations require surgical treatment. Pubertal gynaecomastia often stabilises with time. Observation is a common approach when there are no concerning symptoms.
Addressing underlying contributors can support management. Adjusting medications under medical guidance, or treating relevant medical conditions, may influence the stability of true gynaecomastia.
Lifestyle adjustments may support individuals with pseudogynaecomastia or mixed presentations. Adipose tissue may change with weight management, although glandular tissue generally remains stable.
Medical therapy has been used in selected cases, particularly when changes are recent and associated with discomfort. These treatments are not routinely recommended for all individuals and require assessment of suitability, benefits and limitations.
When true gynaecomastia is persistent and individuals consider surgical options after appropriate assessment, Dr Yezdi Mistry provides treatment for patients in Charlestown, Newcastle and surrounding areas as part of his focused practice in plastic and reconstructive surgery.
Surgical treatment for true gynaecomastia involves direct removal of glandular tissue. When adipose tissue is also present, liposuction techniques may be used to adjust and modify the area for a more even result. The approach chosen depends on individual anatomy and the proportions of glandular and adipose tissue.
Dr Mistry’s specialist training, years of practising and international body contouring education support his approach. Technology such as VASER is used only when suitable for the individual.
All surgery carries risks, including bleeding, infection, changes in nipple sensation, haematoma and scarring. These risks are discussed thoroughly during consultation. Recovery occurs gradually, and follow up appointments support healing over time.
When pseudogynaecomastia persists despite weight stability, individuals may discuss surgical treatment. Liposuction may be considered when adipose tissue forms the main component. Individuals who have experienced significant weight changes may have additional considerations, including skin redundancy.
A combined approach may be discussed when both adipose and glandular components are present. Suitability depends on health, anatomy and goals explored during consultation. Long term results are influenced by general health and weight stability.
Consultations provide time to discuss concerns, review medical history and complete a structured examination. Understanding whether tissue is glandular, adipose or mixed supports clear discussions about possible approaches.
Patients are encouraged to take their time when considering options. Dr Mistry’s specialist training, clinical experience and ongoing professional development support a thorough and informed assessment process. His approach highlights realistic expectations, evidence-based information and respectful communication.
Recovery progresses gradually. Early healing involves rest, wound care and support garments. Follow-up appointments help guide individuals through each stage. Swelling reduces over time, and tissues settle progressively.
In pseudogynaecomastia surgery, similar recovery principles apply. Long-term stability depends on factors such as general health and weight maintenance. Individuals receive information about expected recovery timelines and what changes may occur during healing.
As with all surgery, risks exist and are clearly outlined during consultation.
Yes, some individuals present with both glandular and adipose components. This is known as a mixed pattern and may require a tailored assessment to understand which tissues contribute most to the change. A medical review helps clarify the proportions of each.
Exercise may support general health and influence adipose tissue levels, but glandular tissue does not typically change with physical activity. Individuals often notice that fitness improvements alter some aspects of chest appearance while other features remain stable. This difference can be explored during an examination.
Not always. Many cases can be assessed through history and examination alone, although imaging may be recommended when findings require further clarification. Ultrasound is commonly used when additional detail is helpful.
Certain medications may influence hormone activity, and this can contribute to true gynaecomastia in some individuals. A detailed history helps identify whether a medication may be relevant. Any changes to treatment plans are made in collaboration with the prescribing doctor.
While weight plays a significant role, genetics and individual patterns of adipose distribution also contribute. Some men notice chest fullness even when they have otherwise stable weight. A clinical assessment helps clarify these factors.
Yes, individuals with long-standing glandular tissue may still discuss surgical options if suitable after assessment. The duration of symptoms is one of several factors considered during planning. Surgical decisions are based on examination, health status and personal goals.
Hormonal testing can provide useful information, but not every cause is detectable through laboratory results. Some cases remain idiopathic, meaning no specific cause is identified after appropriate evaluation. Clinical findings remain central to decision-making.
No, asymmetry is common in both true gynaecomastia and pseudogynaecomastia. One side may feel firmer or appear more prominent. This is usually explored duringan examination to understand the pattern more clearly.
Some individuals find that as adipose tissue decreases, the relative prominence of glandular tissue becomes more visible. This does not indicate a new change but reflects the different ways adipose and glandular tissue respond to weight modification. This pattern is often discussed during consultation.
There is no single ideal age. Assessment is suitable at any time when an individual wishes to explore the nature of chest changes or discuss potential management pathways. The approach is adapted to each person’s age, health and medical history.
Dr Mistry established his Charlestown practice after relocating to Newcastle in 2015. The Charlestown Healthcare Hub location provides access for patients from Newcastle and the Hunter region, supporting coordinated care, follow up and ongoing communication.
His background includes FRACS accreditation, specialist training, international body contouring education and years of practising in plastic and reconstructive surgery.
Individuals who notice persistent changes in the chest area or are uncertain about the type of tissue involved may benefit from clinical assessment. Early evaluation supports appropriate planning, whether this involves observation, medical review, lifestyle adjustments or discussion of surgical options.
Dr Mistry provides comprehensive assessment and management for gynaecomastia and pseudogynaecomastia across Charlestown, Newcastle and the Hunter region, guiding individuals through a structured and evidence based process tailored to their circumstances.

Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon based in Newcastle, NSW. With extensive training and experience in both reconstructive and aesthetic surgery, Dr Mistry is committed to providing safe, evidence-based care that is tailored to each patient’s individual needs.
After completing his Fellowship of the Royal Australasian College of Surgeons (FRACS) in Plastic Surgery in 2013, Dr Mistry relocated to Newcastle with his family in 2015. He began his work as a Visiting Medical Officer (VMO) in Plastic and Hand Surgery at John Hunter Hospital before establishing his private practice in 2017. His practice offers a comprehensive range of reconstructive and aesthetic procedures for the breast, body, face, and skin.
Dr Mistry’s approach to patient care is grounded in trust, respect, and open communication. From initial consultation to recovery, he aims to ensure patients feel informed, supported, and comfortable throughout their surgical journey. He is dedicated to maintaining the highest professional and ethical standards in all aspects of his work.
To remain at the forefront of modern surgical techniques, Dr Mistry continues to pursue ongoing professional development both in Australia and internationally. He was Australia’s first delegate at the Body Contouring Academy in Paris, where he received advanced training in body contouring and skin-tightening techniques, including VASER and RENUVION technologies.
Professional Memberships:
Fill in your details and our friendly team will be in touch with you
Please Note: Information provided on Dr Mistry’s website is provided as a basic guide, it does not constitute a diagnosis and should not be taken as medical advice. Any surgical or invasive procedure carries risks.





“I care because it’s my job as a surgeon, as a plastic surgeon, to do the appropriate thing and to give you a good outcome. I want to leave knowing that I can tell a patient, hand on heart, that I did the very best I could and that I looked after them, so when I see them post op later that day or the next morning, that they feel they were in good hands.”
– Dr Yezdi Mistry
Request a Consult