Puffy nipple gynaecomastia is a term used to describe a presentation where the nipple and areola project outward more noticeably than the surrounding chest area. This presentation may first become apparent during adolescence or early adulthood, although some individuals only recognise it later in life. It is common for people to wonder whether this appearance is related to hormone changes, natural development, weight fluctuations or a form of gynaecomastia. Many individuals quietly search for information before seeking professional guidance, often unsure whether what they are observing is typical or whether it warrants medical assessment.
Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon based in Charlestown, NSW, who supports patients across Newcastle, Lake Macquarie and the Hunter region. In his practice, he frequently consults with people seeking clarity about puffy nipple gynaecomastia. His approach is grounded in clinical accuracy, patient-centred communication and evidence-based explanations. This article summarises the type of information he provides during consultations and reflects the balanced, factual tone required within Australian medical advertising regulations.
Puffy nipple gynaecomastia refers to the development of a small amount of glandular breast tissue directly beneath the nipple and areola. This glandular tissue increases projection in this central area. The rest of the chest may remain relatively flat or firm, making the nipple prominence more noticeable.
This presentation represents a mild form of gynaecomastia. Gynaecomastia describes the presence of true glandular breast tissue in males. Glandular tissue is distinct from fat, as it has a firmer texture and tends to form a defined central area beneath the nipple. Even a modest amount can create visible outward projection.
Male breast tissue is responsive to hormonal influences. Variations in the balance between testosterone and oestrogen may stimulate glandular development. Such fluctuations occur naturally during puberty but may also occur later in life due to medication, health conditions or other hormonal factors.


Several factors may contribute to the development of puffy nipple gynaecomastia. Puberty remains one of the most common contexts for its onset. During adolescence, hormone levels shift significantly. Temporary glandular growth is common and often settles over time. Some individuals, however, continue to have a stable area of glandular tissue throughout adulthood.
Hormonal changes in later life can also contribute. Gradual changes in testosterone and oestrogen balance may encourage glandular development. Certain medications influence hormone pathways and may have similar effects in some individuals. Examples include particular anti-androgens, cardiovascular medications, psychiatric medications and anti-retroviral therapies.
Some individuals who use anabolic steroids or certain bodybuilding supplements may notice changes in breast tissue. In some cases, glandular tissue remains long after these substances are discontinued.
Body composition is another factor. Higher fat levels are associated with increased conversion of testosterone into oestrogen within fat cells. While weight loss may reduce fat, established glandular tissue typically does not change with weight reduction. Some individuals only notice the prominence more clearly after becoming leaner.
Various medical conditions that affect hormone regulation may contribute to breast tissue changes. These include thyroid disorders, pituitary abnormalities, testicular conditions, liver disease or rare hormone-producing tumours. When clinically appropriate, investigations can help clarify or exclude these causes.
In many cases, no specific cause is identified. This is known as idiopathic gynaecomastia. It reflects the natural variation in hormone regulation across individuals.
Puffy nipple gynaecomastia is more common than often assumed. Gynaecomastia occurs in a significant proportion of boys during adolescence. Many experience natural reduction in tissue over time, while others continue to observe a stable area of glandular tissue into adulthood.
Individuals with a lean or athletic build often find this prominence more noticeable. This is because the surrounding chest tissues do not mask the glandular projection. Some recognise this appearance during adolescence, while others become aware of it as their body composition changes.
The presentation is considered a variation in how tissue develops. It does not indicate illness. However, assessment may be valuable for individuals who wish to understand the cause or explore potential management options.
A core element of understanding this presentation is differentiating true glandular gynaecomastia from pseudogynaecomastia, which refers to fat-related chest fullness.
Glandular breast tissue is firmer and forms a distinct area beneath the nipple. It does not typically reduce with weight loss. In contrast, fat is softer and more evenly distributed across the chest. Fat-related fullness usually decreases with weight reduction.
Many individuals have a combination of both tissue types. For those with primarily glandular tissue, weight change alone does not alter nipple prominence. Identifying the tissue characteristics guides whether conservative or surgical management may be appropriate.
Most cases of puffy nipple gynaecomastia are benign and remain stable for many years. However, certain features warrant timely medical review. These include sudden enlargement, nipple discharge, new skin changes, a firm lump on one side, or persistent new tenderness. These symptoms require assessment to exclude other conditions.
For individuals with long-standing, stable tissue who would like clarity on its nature, a consultation provides reassurance and guidance.
During a consultation with Dr Mistry, the assessment process begins with a detailed medical history. This covers when the prominence was first noticed, whether it has changed, any associated symptoms, medication use, supplement use, family history and overall health. Understanding the timeline and context helps identify whether further testing may be appropriate.
A physical examination follows. Dr Mistry assesses the characteristics of the tissue directly beneath the nipple, the surrounding chest, skin features and overall proportions. True glandular tissue produces a distinct feel and distribution, while fat behaves differently on examination.
If the presentation appears benign and consistent with typical gynaecomastia, further testing may not be required. If the findings are unclear or if there are factors suggesting a hormonal or medical cause, blood tests may be recommended. These may assess hormone levels, liver and thyroid function or other relevant markers. Ultrasound may be arranged when further clarification is useful.
This structured assessment approach supports accurate diagnosis and helps patients understand their available pathways.
Management varies depending on the cause, stability and impact of the glandular tissue. Some individuals require no treatment and simply wish to understand what is responsible for the appearance. For adolescents or young adults, observation may be appropriate because their glands may still be changing.
When an underlying medical or medication-related cause is identified, addressing that cause is the first step. This may involve collaboration with a general practitioner or specialist.
For individuals whose tissue remains unchanged and who feel the prominence affects their day-to-day preferences or comfort, surgical management may be considered. Decisions regarding surgery are personal and require assessment of individual goals, anatomy and health considerations. Surgery is not necessary for everyone and is only recommended when it is appropriate for the individual’s situation.
Surgical treatment focuses on removing the glandular tissue beneath the nipple. A small incision is typically placed along the border of the areola. Through this incision, the glandular tissue responsible for the projection is carefully removed. The aim is to modify the shape of the nipple and surrounding area while preserving normal anatomical features.
When fat is also present, liposuction may be used to change the shape of the surrounding chest tissue. VASER-assisted liposuction may be incorporated when appropriate. The choice of technique depends on the individual’s anatomy and clinical needs.
The objective of surgery is to reduce glandular prominence and support a balanced chest appearance. Surgical planning takes into account the amount of glandular tissue, surrounding tissues, skin characteristics and the person’s overall health.
Recovery after gynaecomastia occurs gradually and differs among individuals. A compression garment is usually recommended to support the chest and help control swelling. Some discomfort may be experienced in the early period. This is managed with appropriate medication. Swelling and bruising reduce over several weeks.
Light activities may resume early, with more physically demanding activities gradually reintroduced according to postoperative guidance. In Dr Mistry’s practice, individuals receive written postoperative instructions that detail wound care, garment use, activity recommendations and follow-up appointments.
The position and appearance of the nipple and surrounding tissue evolve over time as swelling settles and tissues adjust. Final results take several months to develop.
Disclaimer: The outcomes shown are specific to those patients and may not reflect the results experienced by others, as individual outcomes can vary due to a range of factors.

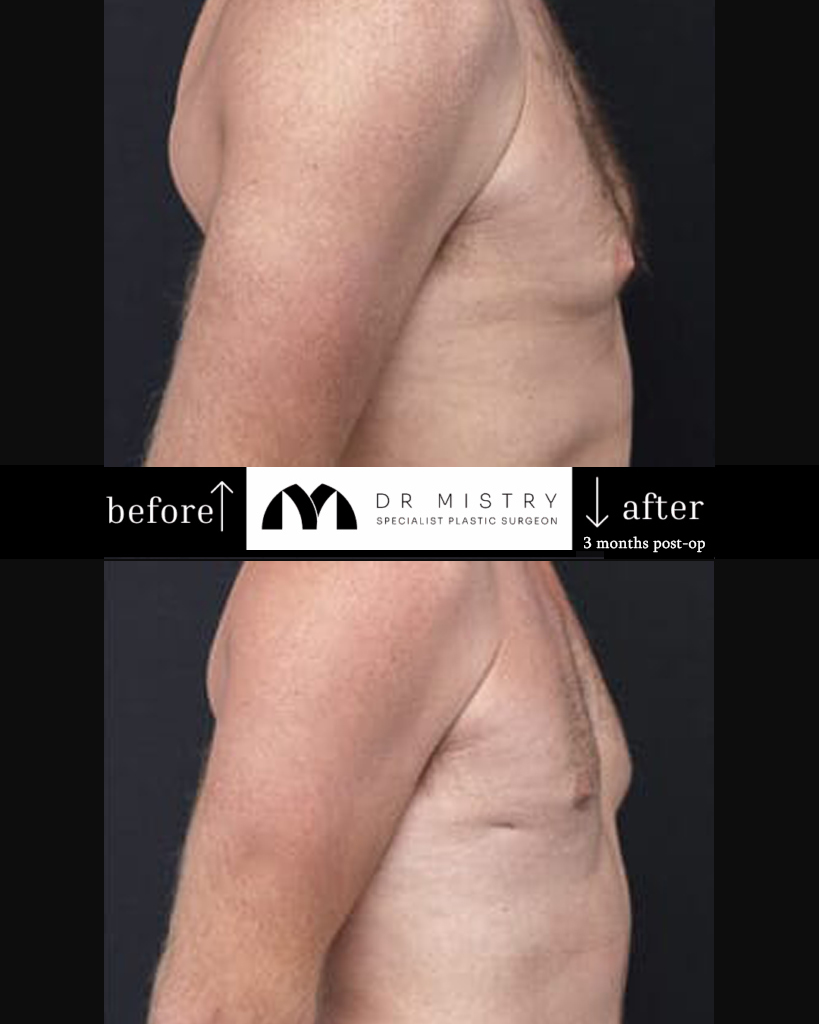
Each person presents with unique anatomical features. The firmness of glandular tissue, the thickness of the surrounding tissues, skin characteristics and overall chest proportions vary significantly. These factors influence both surgical planning and the expected changes.
Surgery aims to modify the tissue in a predictable and clinically appropriate way, not to create idealised or guaranteed outcomes. The final appearance reflects the original tissue characteristics, the extent of glandular tissue and individual healing patterns. During consultation, Dr Mistry discusses realistic expectations based on the person’s anatomy and medical history.
Glandular tissue removed during surgery does not typically return. However, future hormonal changes, significant weight changes or certain medications can influence the appearance of the chest. Good general health helps maintain stability.
Many individuals live comfortably with this presentation. Others would like clarity about its cause or wish to explore management pathways. Seeking assessment may be helpful for those who have noticed recent changes, have long-standing uncertainty about the cause or simply want professional guidance.
Some individuals gain reassurance that their presentation is benign and stable. Others decide to explore surgical pathways after discussing the options. Dr Mistry’s role is to provide balanced information, outline recognised risks and support informed decision-making without suggesting that treatment is necessary.
Yes, many individuals experience a stable presentation that does not cause medical concerns. In these cases, the tissue simply reflects the way breast glands developed and remained over time.
Puberty is a common time for this presentation to begin, but not the only one. Some individuals develop glandular prominence due to medications, health conditions or natural variation in hormone patterns during adulthood.
Exercise can change overall body composition, but it does not remove glandular tissue. Some individuals may notice the area more clearly as surrounding fat decreases with increased fitness.
In most individuals, the presentation does not change nipple sensation. If sensation changes, it is usually related to other factors, and assessment may be helpful for clarity.
Yes, although symmetry is common, some individuals experience more noticeable prominence on one side. When this occurs, assessment is recommended to confirm the tissue characteristics.
Not necessarily. While increased fat can influence the surrounding area, the glandular component may appear more or less noticeable depending on overall chest changes.
Removed glandular tissue does not usually return. However, hormonal changes, significant weight changes or certain medications may influence the appearance of the chest in the future.
Diet alone is not known to cause glandular growth. However, body weight changes may influence how pronounced the area appears in some individuals.
Some individuals report mild sensitivity when pressure is applied to the area. This varies from person to person and depends on the amount and firmness of the glandular tissue.
Assessment can occur at any age if the individual has concerns or notices changes. Evaluation is particularly helpful when the presentation is new, evolving or associated with unusual symptoms.
Individuals who would like to understand the cause of their puffy nipple gynaecomastia or who are considering management options are welcome to attend Dr Mistry’s practice at the Charlestown Healthcare Centre. During a gynaecomastia consultation, Dr Mistry reviews the individual’s history, examines the area, determines whether further investigation is needed and outlines appropriate management pathways.
His goal is to support patient understanding, provide accurate information and guide individuals through their options in a considered and evidence-based manner.

Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon based in Newcastle, NSW. With extensive training and experience in both reconstructive and aesthetic surgery, Dr Mistry is committed to providing safe, evidence-based care that is tailored to each patient’s individual needs.
After completing his Fellowship of the Royal Australasian College of Surgeons (FRACS) in Plastic Surgery in 2013, Dr Mistry relocated to Newcastle with his family in 2015. He began his work as a Visiting Medical Officer (VMO) in Plastic and Hand Surgery at John Hunter Hospital before establishing his private practice in 2017. His practice offers a comprehensive range of reconstructive and aesthetic procedures for the breast, body, face, and skin.
Dr Mistry’s approach to patient care is grounded in trust, respect, and open communication. From initial consultation to recovery, he aims to ensure patients feel informed, supported, and comfortable throughout their surgical journey. He is dedicated to maintaining the highest professional and ethical standards in all aspects of his work.
To remain at the forefront of modern surgical techniques, Dr Mistry continues to pursue ongoing professional development both in Australia and internationally. He was Australia’s first delegate at the Body Contouring Academy in Paris, where he received advanced training in body contouring and skin-tightening techniques, including VASER and RENUVION technologies.
Professional Memberships:
Fill in your details and our friendly team will be in touch with you
Please Note: Information provided on Dr Mistry’s website is provided as a basic guide, it does not constitute a diagnosis and should not be taken as medical advice. Any surgical or invasive procedure carries risks.





“I care because it’s my job as a surgeon, as a plastic surgeon, to do the appropriate thing and to give you a good outcome. I want to leave knowing that I can tell a patient, hand on heart, that I did the very best I could and that I looked after them, so when I see them post op later that day or the next morning, that they feel they were in good hands.”
– Dr Yezdi Mistry
Request a Consult