Gynaecomastia, also spelled Gynecomastia in American English, refers to the benign enlargement of glandular breast tissue in males. Although many people think of this condition as uncommon, it is in fact one of the more frequent reasons men seek medical advice for changes in the chest area. It can occur at different ages and for a range of reasons, many of which relate to variations in hormone activity within the body. Understanding the underlying contributors is important because gynaecomastia is not a diagnosis by itself but rather a physical sign that can arise in different developmental, medical, or lifestyle situations. This comprehensive article reflects the educational style of Dr Yezdi Mistry, Specialist Plastic and Reconstructive Surgeon based in Charlestown, NSW, and outlines why gynaecomastia occurs, what may influence it, and why evaluation with a qualified doctor is important when changes in chest tissue develop.
Dr Yezdi Mistry cares for men from Charlestown, Newcastle, and the Hunter region who seek clarity regarding enlarged male breast tissue. His approach is grounded in detailed assessment, clear communication, and evidence-based practice. As with all medical conditions, individual evaluation is necessary, and this article is intended to provide general information rather than personalised medical advice.
Understanding the mechanisms behind gynaecomastia requires an appreciation of how male breast tissue responds to hormonal signals. Male breast tissue is sensitive to the relationship between androgens such as testosterone and oestrogens, which are present in smaller but meaningful amounts. When this balance changes, whether through reduced androgen activity, increased oestrogen activity, or increased sensitivity within the breast tissue, the glandular component may enlarge. These hormonal variations differ among individuals, and often no single factor explains the change. This overview explores physiological causes, medications, endocrine conditions, systemic health disorders, weight related factors, and idiopathic cases where no specific cause is identified.
Gynaecomastia arises from the proliferation of glandular breast tissue rather than fat. This distinction is important because some men develop increased chest prominence primarily due to fat accumulation. When fat rather than glandular tissue is the main contributor, the pattern is often referred to as pseudo-gynaecomastia. In many individuals, both components contribute to the presentation, and clinical examination helps clarify these patterns.
Gynaecomastia may affect one or both sides of the chest. The enlargement can vary in firmness and distribution. Some men notice a firm area of tissue beneath the nipple, while others experience a broader pattern that blends with chest fat. These variations highlight the importance of a personalised clinical evaluation before considering management options.
Gynaecomastia may develop during normal life stages, as a result of medications, or due to an underlying medical condition influencing hormone activity. In some situations, the enlargement settles, particularly during adolescence, while in others it persists. A Specialist Plastic and Reconstructive Surgeon like Dr Yezdi Mistry supports individuals in clarifying the type of tissue present, assessing whether the condition may change over time, and discussing management options when appropriate.



Physiological gynaecomastia occurs at predictable stages of life due to temporary changes in hormone levels. These stages include newborn infancy, adolescence, and older adulthood. In these situations, the enlargement reflects normal hormonal variations rather than underlying disease.
In newborn males, temporary breast tissue enlargement may occur due to maternal oestrogen exposure before birth. This type of gynaecomastia usually settles within several weeks, demonstrating how sensitive male breast tissue can be to hormonal changes.
Adolescent gynaecomastia is more widely recognised. During puberty, hormone levels fluctuate as the body progresses toward adulthood. Testosterone levels rise, but so do oestrogen levels, and the relationship between these hormones may shift frequently. This temporary variation can result in a firm disc of glandular tissue beneath the nipple. In most adolescents, the enlargement settles as hormone levels stabilise. Some young men, however, experience persistent tissue, influenced by individual biological differences.
In older men, testosterone levels gradually decrease over time. This may be accompanied by increased conversion of androgens to oestrogens in fat tissue, particularly in individuals with higher body fat levels. These variations can influence hormonal balance and encourage breast tissue growth. Age-related gynaecomastia may develop slowly and can be influenced by general health, medications, or broader metabolic changes.
A significant number of gynaecomastia cases arise from medications and substances that influence hormone balance. Because breast tissue responds to hormonal signalling, medications that reduce testosterone, increase oestrogen activity, or affect hormone receptors can contribute to glandular enlargement.
Some medications used for prostate health reduce the effect of androgens in the body. When androgen activity reduces, oestrogen activity may become relatively more dominant, encouraging glandular tissue growth. Certain medications used for heart conditions have been associated with gynaecomastia in some individuals. Older medications for reflux or ulcer disease have also been linked to hormonal changes when used at high doses, while some psychiatric medications may influence hormone pathways that interact with breast tissue.
Non-medical substances such as anabolic androgenic steroids may also contribute. During use, androgen levels rise, but the body often reduces its natural testosterone production. When steroid use stops, testosterone levels may drop, leading to an environment that supports breast tissue growth. Alcohol consumption and some recreational drugs may influence hormone metabolism or liver function, indirectly contributing to gynaecomastia.
Medication-related gynaecomastia highlights the importance of a complete medical history. Dr Yezdi Mistry routinely discusses prescribed medications, over-the-counter products, supplements, and any past or current use of non-medical substances. This supports understanding of whether changes may settle after medication adjustments or whether they are likely to persist.
Endocrine conditions affect hormone production and regulation, making them an important group of contributors to gynaecomastia.
Hypogonadism, which involves reduced testosterone production, is one of the more frequent endocrine contributors. Causes may originate in the testes or result from reduced hormonal signalling from the pituitary gland. When testosterone levels fall, breast tissue may respond even if oestrogen levels remain stable. Some genetic conditions, such as Klinefelter syndrome, also involve reduced testicular function and may present with gynaecomastia.
Thyroid overactivity influences hormone circulation. In hyperthyroidism, increased metabolic activity affects hormone-binding proteins, altering how hormones interact with tissues. This environment may encourage glandular breast tissue growth. Men with hyperthyroidism often have additional symptoms that help guide assessment.
Androgen resistance conditions involve situations where the body produces androgens, but tissues respond differently than expected. Breast tissue may remain sensitive to small amounts of oestrogen. Rare conditions affecting aromatase enzymes, which convert androgens to oestrogens, can also contribute.
When an endocrine condition is suspected, Dr Yezdi Mistry may arrange blood tests to assess hormone levels, pituitary function, and other markers. This supports the identification of conditions that require medical management before any discussion of procedural options.
Systemic medical conditions may influence hormone metabolism or cause direct hormone production, contributing to gynaecomastia. Although less common than physiological or medication-related causes, these contributors are clinically important.
Liver disease is one recognised contributor. The liver plays a central role in hormone metabolism. When liver function is reduced, oestrogen levels may rise, or androgen metabolism may change. Chronic liver disease may also be associated with metabolic differences that affect hormonal pathways.
Chronic kidney disease may contribute to gynaecomastia, particularly in advanced stages. Medications used in kidney disease may also influence hormone activity. Malnutrition and systemic illnesses can affect hormone production and metabolism.
Tumour-related gynaecomastia is uncommon but important to identify promptly. Certain tumours produce hormones that stimulate breast tissue, such as human chorionic gonadotropin or oestrogens. Testicular tumours are among the better recognised examples, and men experiencing chest changes along with testicular discomfort or swelling should seek timely assessment. Adrenal tumours and other hormone-producing tumours may also contribute. Identifying these conditions early supports appropriate medical care.
When men present with new or rapid breast tissue enlargement, Dr Yezdi Mistry may collaborate with general practitioners, endocrinologists, or other specialists to facilitate a comprehensive evaluation.


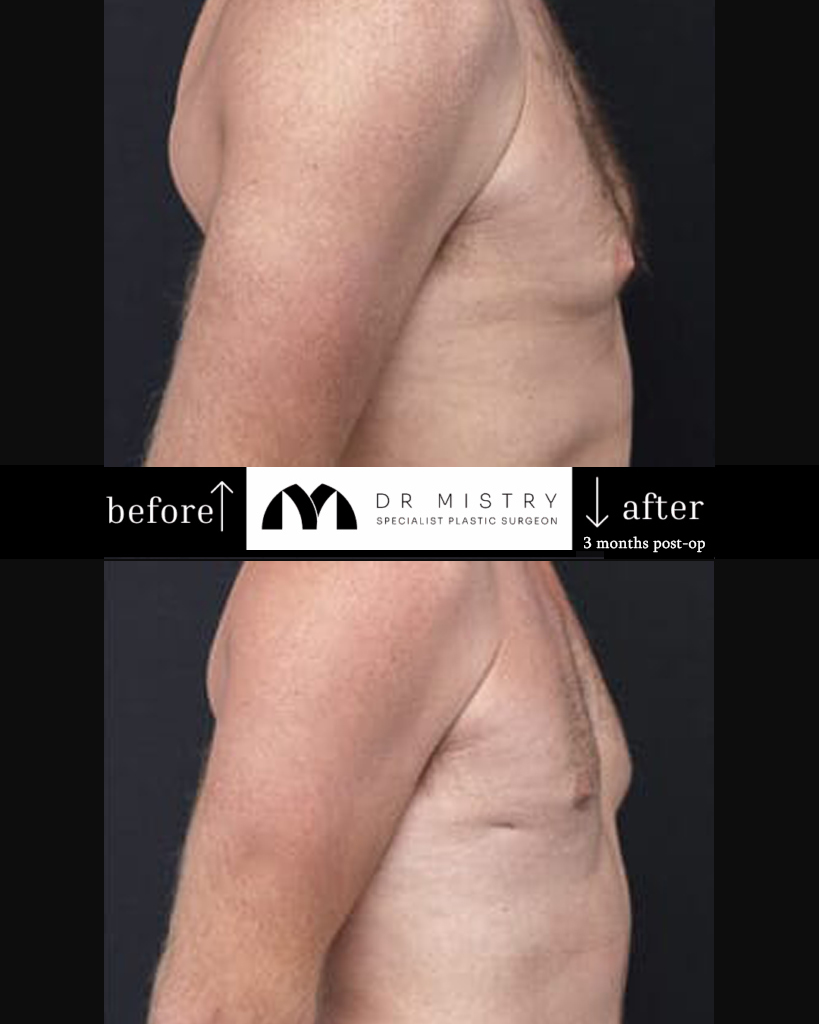
Disclaimer: The outcomes shown are specific to those patients and may not reflect the results experienced by others, as individual outcomes can vary due to a range of factors.
Obesity contributes to chest changes in several ways, and many patients ask whether being overweight can directly cause gynaecomastia. Increased fat in the chest can give the appearance of enlargement even when glandular tissue is minimal. This is known as pseudo-gynaecomastia. Higher body fat levels also increase aromatase activity, converting androgens to oestrogens, which may encourage glandular tissue development. Many individuals experience both fat and glandular components.
A clinical assessment helps distinguish between these tissue types. Men may notice soft fullness, firmer tissue beneath the nipple, or asymmetry. Dr Yezdi Mistry performs detailed examinations to guide appropriate recommendations based on the tissue present.
A substantial proportion of men experience gynaecomastia without an identifiable cause. These cases are described as idiopathic. This does not diminish the validity of the symptoms. Instead, current medical testing does not identify a specific mechanism. Idiopathic Gynaecomastia may remain stable or progress gradually over time.
Assessment focuses on ruling out identifiable causes and understanding the characteristics of the tissue. Many patients seek guidance because the change has been present for years or because they are uncertain about its origin. Consultation with Dr Yezdi Mistry provides an opportunity to discuss history, concerns, and next steps.
Assessment is central to understanding gynaecomastia and planning appropriate management. Dr Yezdi Mistry conducts comprehensive evaluations in his Charlestown practice, focusing on history, examination, and contributing factors.
Assessment includes discussion of when the change began, how it has progressed, and whether there is discomfort or associated symptoms. Medical background, medications, lifestyle factors, and endocrine history are reviewed. Physical examination helps clarify the proportion of glandular tissue, fat distribution, skin characteristics, and symmetry.
Further investigations may be recommended. These may include blood tests to evaluate hormone levels or organ function. Imaging, such as ultrasound may be arranged to clarify tissue composition or assess the testes when indicated. This thorough evaluation supports informed decision-making.
Gynaecomastia may influence how some individuals feel in day-to-day settings, prompting them to seek medical information. Men often seek guidance because they feel uncertain about the cause or because the change has been present for some time. Providing clear explanations supports informed discussions.
In some cases, individuals have noted a shift in how they view certain aspects of their appearance after better understanding the contributing factors. This can help guide decisions about future management.
Gynaecomastia is a physical sign with many potential contributors, not a single condition. Accurate diagnosis supports appropriate care and helps determine whether the change may settle, remain stable, or require further evaluation. For example, adolescent gynaecomastia may settle as hormone levels stabilise, medication-related cases may change after adjustments, and endocrine conditions often require targeted medical treatment.
Accurate diagnosis also supports patient safety by identifying uncommon but important causes such as hormone-producing tumours. Systemic diseases and endocrine disorders may require medical attention beyond the chest tissues alone.
Dr Yezdi Mistry draws on clinical experience, specialist training, and years of practising plastic and reconstructive surgery to support patients through this process. Once the underlying contributors are understood, a balanced discussion about suitable management pathways can take place.
Men in Charlestown, Newcastle, and the Hunter region commonly seek information about chest changes. Reasons vary, including changes after adolescence, gradual changes with age, or uncertainty about the cause.
Dr Yezdi Mistry’s practice in the Charlestown Healthcare Hub provides a setting where patients can discuss concerns privately. Consultations focus on clear communication, individualised guidance, and evidence-based information. As a surgeon with extensive knowledge, clinical experience, and specialist training, Dr Mistry supports patients in understanding the type of tissue present and discussing potential next steps when appropriate.
Lifestyle factors may influence hormone levels, body composition, and general health. Weight changes, alcohol use, and metabolic health can affect breast tissue behaviour. Individuals who experience fluctuations in weight may notice changes in chest appearance over time. Supporting general health may contribute to a more stable hormone balance.
Working with medical practitioners to address contributors such as weight, alcohol use, or endocrine disorders is an important component of long-term well-being. While glandular tissue may not always resolve, improving overall health may support broader medical outcomes if treatment is later considered.
Men may benefit from medical assessment when they notice new or unexplained chest changes, when there is discomfort, or when the cause is unclear. Rapid changes, asymmetry, or symptoms such as testicular discomfort should prompt timely evaluation. Even long standing changes may warrant assessment to clarify the type of tissue present.
During a consultation at his Charlestown practice, Dr Yezdi Mistry reviews medical history, examines the chest, considers potential contributors, and outlines any investigations that may be helpful. This supports informed decision-making and evidence-based discussion about future care.
Gynaecomastia has many possible contributors. Physiological changes during infancy, adolescence, and older adulthood may influence hormone balance. Medications, endocrine conditions, systemic diseases, and lifestyle factors may contribute to more persistent cases. Some individuals experience Gynaecomastia without an identifiable cause, known as idiopathic gynaecomastia. Understanding these contributors helps guide assessment and management.
Dr Yezdi Mistry, Specialist Plastic and Reconstructive Surgeon, provides a detailed evaluation for men in Charlestown, Newcastle, and the Hunter region seeking clarity regarding male breast tissue changes. His approach focuses on personalised assessment, evidence-based recommendations, and clear communication about available pathways. For individuals experiencing chest changes, consultation supports understanding of underlying contributors and discussion of suitable options.

Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon based in Newcastle, NSW. With extensive training and experience in both reconstructive and aesthetic surgery, Dr Mistry is committed to providing safe, evidence-based care that is tailored to each patient’s individual needs.
After completing his Fellowship of the Royal Australasian College of Surgeons (FRACS) in Plastic Surgery in 2013, Dr Mistry relocated to Newcastle with his family in 2015. He began his work as a Visiting Medical Officer (VMO) in Plastic and Hand Surgery at John Hunter Hospital before establishing his private practice in 2017. His practice offers a comprehensive range of reconstructive and aesthetic procedures for the breast, body, face, and skin.
Dr Mistry’s approach to patient care is grounded in trust, respect, and open communication. From initial consultation to recovery, he aims to ensure patients feel informed, supported, and comfortable throughout their surgical journey. He is dedicated to maintaining the highest professional and ethical standards in all aspects of his work.
To remain at the forefront of modern surgical techniques, Dr Mistry continues to pursue ongoing professional development both in Australia and internationally. He was Australia’s first delegate at the Body Contouring Academy in Paris, where he received advanced training in body contouring and skin-tightening techniques, including VASER and RENUVION technologies.
Professional Memberships:
Fill in your details and our friendly team will be in touch with you
Please Note: Information provided on Dr Mistry’s website is provided as a basic guide, it does not constitute a diagnosis and should not be taken as medical advice. Any surgical or invasive procedure carries risks.





“I care because it’s my job as a surgeon, as a plastic surgeon, to do the appropriate thing and to give you a good outcome. I want to leave knowing that I can tell a patient, hand on heart, that I did the very best I could and that I looked after them, so when I see them post op later that day or the next morning, that they feel they were in good hands.”
– Dr Yezdi Mistry
Request a Consult