Gynaecomastia is a condition that many men experience at different stages of life, and it often raises questions about why it develops and whether body weight plays a role. Men across Charlestown, Newcastle and the Hunter region commonly notice gradual or unexpected changes in the chest during day-to-day activities, exercise or weight fluctuations. For some, it becomes important to understand if these changes relate to fatty tissue, glandular tissue or a combination of both.
Dr Yezdi Mistry, Specialist Plastic and Reconstructive Surgeon is based in Charlestown, NSW. The purpose of this article is to explain how weight may influence gynaecomastia, describe the typical features that men may observe and outline potential physical effects. The information is general and intended to guide understanding rather than replace personalised medical advice.
Gynaecomastia refers to the benign enlargement of the glandular breast tissue in men. This glandular tissue sits beneath the nipple areolar complex and has a firmer, more structured quality compared with fatty tissue. Its development is influenced by the balance between androgens and oestrogen. When this balance changes, the glandular tissue may become more noticeable.
It is important to distinguish between glandular enlargement and fullness created by fatty tissue. Increased body fat across the chest can lead to a softer, more diffuse form of fullness known as pseudogynaecomastia. Both conditions can appear similar when viewed in a mirror or when wearing fitted clothing, and many men experience both at the same time because excess fat can sit over existing glandular tissue.
Although gynaecomastia itself is generally benign, identifying the contributing factors can be valuable. Hormonal changes, physiological stages of life, medical conditions, medication use and weight can all influence the development of glandular tissue. Understanding these distinctions helps men better interpret the nature of the changes they observe.


Being overweight does not automatically cause glandular gynaecomastia, but increased body fat levels can contribute to chest changes in several interconnected ways. Hormone activity, fat distribution, metabolic factors and individual sensitivity all play a role.
Fatty tissue contains aromatase, an enzyme that converts testosterone into oestradiol. As body fat increases, aromatase activity may also increase, potentially contributing to a shift in the hormone balance. Not all men experience the same degree of hormonal change, but for some individuals this shift may be enough to influence glandular tissue.
Weight gain can also affect the distribution of fat across the chest. Men with a higher body mass index often notice soft, diffuse fullness in the chest area. This is different from glandular tissue, which tends to remain central beneath the nipple areolar complex. Men may therefore experience enlargement from fat, glandular tissue or a combination.
Medical literature consistently notes a higher prevalence of male breast enlargement in individuals with elevated body mass index. This association highlights how weight can interact with other biological factors but does not mean that weight is the sole cause for all men. Men with healthy body weight can also develop gynaecomastia due to other hormonal or medical influences.
Weight loss may support a reduction in fatty tissue across the chest, although longstanding glandular tissue usually remains unchanged. Understanding this difference can help guide expectations about which aspects of chest fullness may respond to lifestyle adjustments and which may not.
Men often first notice chest changes during daily routines such as dressing, showering or engaging in physical activity. Recognising typical features can help distinguish between glandular and fatty tissue.
Gynaecomastia commonly presents as a firm, rubbery area of tissue directly beneath the nipple areolar complex. It may be tender during earlier stages and can occur on one or both sides. When it occurs on one side only, the difference may be visible in the mirror or felt when comparing both sides of the chest. The tissue generally does not fluctuate significantly with short term weight changes.
Pseudogynaecomastia feels softer and more diffuse. Men often notice that the fullness extends towards the outer chest or into the axillary fold. This type of tissue tends to change more noticeably with weight gain or weight loss and typically does not cause tenderness.
Certain signs require prompt medical assessment. These include firm or irregular lumps, sudden enlargement, nipple discharge, tethering of the skin, nipple inversion or swelling of nearby lymph nodes. These features are not typical of benign gynaecomastia and should be reviewed by a general practitioner. These signs are not usually related to weight changes, making timely assessment important.
Understanding these patterns helps men identify when changes may relate to weight distribution or when further evaluation is appropriate.
Although weight is a common factor discussed in relation to male breast enlargement, gynaecomastia can develop for many reasons. Physiological stages of life, hormone fluctuations, medical conditions and medication use all contribute in various ways.
Newborn boys may experience temporary breast tissue enlargement due to the influence of maternal hormones. This typically resolves within the first few weeks of life.
Adolescence is one of the most common periods for glandular tissue to develop. Hormonal fluctuations during puberty can temporarily shift the androgen to oestrogen balance. Many adolescent boys experience a degree of glandular tissue during this time and, for most, it settles naturally over one to two years. A small number may have persistent tissue that continues into adulthood.
In adult men, gradual age related changes in hormones, shifts in body composition and changes in how the liver processes hormones can contribute to glandular development. These influences vary among individuals and often develop gradually.
Medical conditions such as hypogonadism, hyperthyroidism, chronic liver disease, chronic kidney disease and hormone-producing tumours can also affect hormone balance. When gynaecomastia is linked to an underlying condition, evaluation and management of the primary issue may influence the overall pattern.
Some medications can contribute to hormonal changes in men. These include certain prostate treatments, anti androgen medications, some antidepressants, antipsychotics, anti ulcer medications and medications used in specific chronic health conditions. Men who notice chest changes after starting new medication may find it helpful to discuss this with their prescribing doctor.
Weight can influence hormone regulation in several ways. Adipose tissue is an active metabolic tissue that interacts with hormone production, inflammation and endocrine pathways.
As body fat increases, aromatase activity may increase. Aromatase converts androgens into oestrogens. This change may contribute to a subtle shift in the hormone balance, which in some men may influence breast tissue.
Sex hormone binding globulin levels can also be affected by higher body fat. This protein regulates the amount of testosterone available in the bloodstream. Reduced levels may influence the hormonal environment and potentially contribute to glandular stimulation in susceptible individuals.
Metabolic factors such as insulin resistance and variations in leptin, which are more common in individuals with higher body fat, can influence hormone pathways indirectly. These factors do not directly cause gynaecomastia but may contribute to conditions that affect hormone balance.
Understanding these mechanisms helps explain why weight changes sometimes coincide with changes in glandular tissue and why glandular tissue may remain even when weight decreases.
Gynaecomastia can influence daily activities in different ways depending on the amount of glandular tissue, the presence of associated sensitivity and the individual’s routine.
Some men experience sensitivity across the nipple areolar complex, particularly when glandular tissue is hormonally active. This sensitivity may be noticed during exercise, upper body movements or contact with clothing.
The presence of glandular or fatty tissue in the chest may also influence clothing preferences. Some men choose looser shirts or layered clothing. Others feel more aware of their chest during sports, swimming or settings where the upper body is exposed. These experiences vary widely between individuals and are not necessarily related to the degree of enlargement.
Pseudogynaecomastia presents differently, with softer and more diffuse tissue that may move more during activity. Some men describe a sense of fullness or weight in the chest area rather than localised sensitivity. Weight changes may influence these sensations over time.
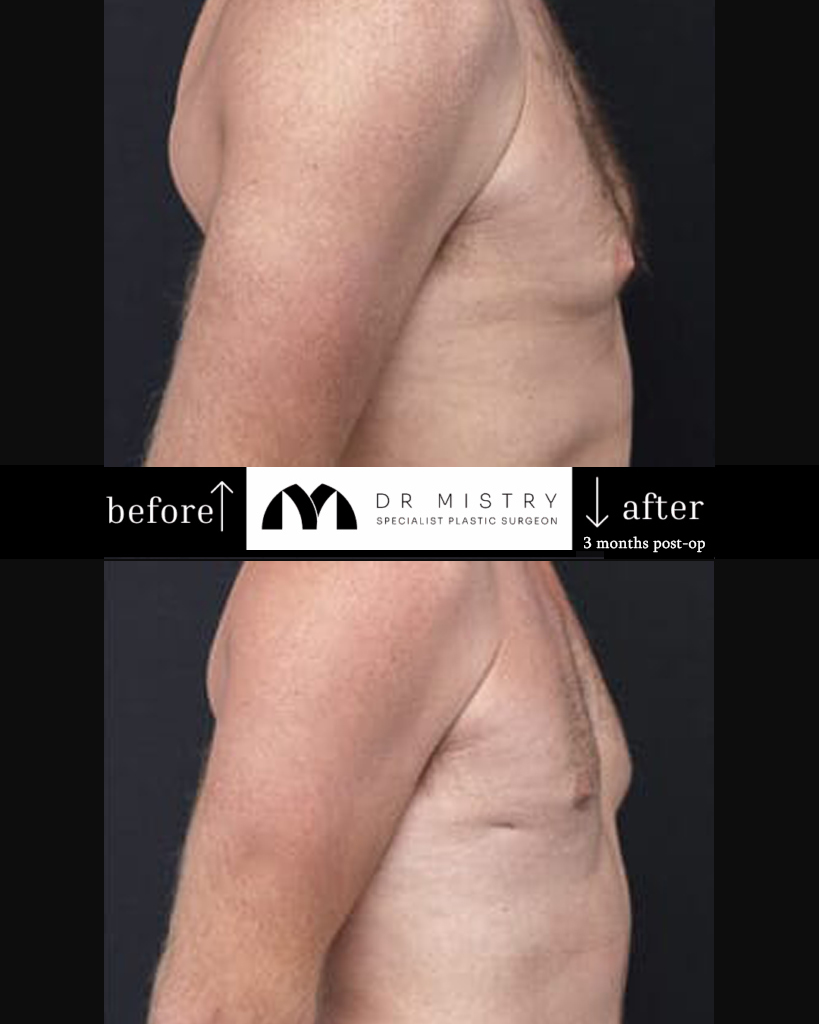
Disclaimer: The outcomes shown are specific to those patients and may not reflect the results experienced by others, as individual outcomes can vary due to a range of factors.

Any new or persistent change in the male breast region may benefit from medical assessment, particularly when the cause is unclear. A general practitioner can assess the area, review medical history, examine potential contributing factors and arrange tests where appropriate.
Assessment can be useful when glandular enlargement persists beyond adolescence, continues despite lifestyle adjustments or is associated with tenderness that does not settle. It is particularly important when concerning signs are present such as nipple discharge, sudden enlargement, skin tethering, nipple inversion or firm irregular masses.
Men who have made health related changes such as weight adjustments and continue to notice persistent tissue may find a medical review helpful in understanding the nature of the tissue and whether further assessment is appropriate.
Lifestyle considerations can play an important role in managing fatty chest fullness for men with higher body weight. Gradual weight loss achieved through accessible, balanced nutrition and physical activity may support a reduction in fatty tissue across the chest and contribute to broader health improvements.
However, glandular tissue behaves differently to fatty tissue. Longstanding glandular enlargement typically remains even when body weight decreases. In some individuals, weight loss may make glandular tissue more noticeable because the surrounding fat reduces. This can prompt some men to seek medical discussion once lifestyle factors have been addressed.
Understanding these differences helps men interpret the changes they notice and consider whether further evaluation may be beneficial.
Clinical assessment aims to clarify whether chest changes represent glandular tissue, fatty tissue or both. The process generally begins with a detailed history to identify contributing factors such as onset, duration, associated symptoms, medication use and relevant medical conditions.
The physical examination allows the clinician to distinguish between the firmness of glandular tissue and the softer, more diffuse nature of fatty tissue. Some individuals have a combination of both, and careful assessment helps identify the proportions.
If further clarity is required, investigations may be arranged. These may include blood tests to assess hormone levels or evaluate liver, kidney or thyroid function. Imaging such as ultrasound may be considered in selected circumstances. These steps are tailored to the individual’s situation rather than applied routinely to all cases.
At his Charlestown practice, Dr Yezdi Mistry draws on his clinical experience, specialist training and years of practising in Plastic and Reconstructive Surgery to assess gynaecomastia. His consultations focus on clear explanations, individualised evaluation and an approach centered on the patient’s circumstances and questions.
Yes. When men lose weight, the reduction in surrounding fatty tissue can make existing glandular tissue feel more defined. This can create the impression of new or increased tissue even though the glandular component may have remained the same.
Exercise cannot directly reduce glandular tissue, although it can modify overall body composition and change how the chest appears. Some men notice that as muscle increases, the relative prominence of glandular tissue becomes easier to feel.
Yes. Fat distribution is not always symmetrical, and some men gain or lose fat unevenly across the chest. This can create a difference in appearance or feel even without a glandular component.
Diet alone is unlikely to directly stimulate glandular tissue, but nutritional choices can influence body weight and metabolic patterns. These changes may indirectly contribute to the hormonal environment that affects breast tissue in some men.
Yes. Age related shifts in hormone balance may make existing glandular tissue more noticeable or persistent over time. This is separate from fatty changes and may occur regardless of weight variation.
Yes. When there is a significant amount of fatty tissue, glandular tissue can feel obscured or blended into the surrounding area. Clinical assessment can help differentiate between the two.
Men with longstanding glandular tissue often find that weight loss mainly affects the fatty component, while the glandular tissue remains. This can result in a different overall appearance even after meaningful lifestyle adjustments.
Yes. Some medications influence hormone pathways, and higher body weight can affect how these medications are metabolised. The combination may make glandular tissue more noticeable in certain individuals.
Short term changes in weight can influence how soft tissue feels, particularly in individuals with a higher proportion of fatty tissue. These fluctuations do not typically affect glandular tissue but may alter how the area is perceived.
Yes. The way the shoulders and chest are positioned can influence how tissue rests against the body. This can make chest fullness appear more or less noticeable in different positions or clothing styles.
Gynaecomastia can follow different patterns depending on its cause. Pubertal gynaecomastia often resolves as hormones stabilise. Weight related pseudogynaecomastia may decrease as weight reduces, although glandular tissue beneath the fat may remain unchanged.
Longstanding glandular tissue in adults may become more fibrous over time, which means it is less affected by hormonal fluctuations or lifestyle changes. Understanding these patterns can help men determine whether monitoring, lifestyle adjustment or further evaluation may be suitable for their situation.
Men in the Newcastle and Hunter region often seek a specialist consultation to better understand the features of their gynaecomastia, clarify the type of tissue present and discuss long term expectations or possible male reduction surgery. At his Charlestown practice, Dr Yezdi Mistry provides comprehensive consultations for individuals seeking information about male chest changes.
As a Specialist Plastic and Reconstructive Surgeon with extensive experience, advanced training and a focused practice in male chest procedures, Dr Mistry performs detailed assessments that consider medical history, physical findings and contributing factors. During the consultation, he discusses features of the chest, reviews potential influences and explains which aspects may or may not respond to weight adjustments or lifestyle modifications.
Throughout the process, Dr Mistry maintains an evidence based, patient centred approach that supports individuals in understanding their condition and making informed decisions.

Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon based in Newcastle, NSW. With extensive training and experience in both reconstructive and aesthetic surgery, Dr Mistry is committed to providing safe, evidence-based care that is tailored to each patient’s individual needs.
After completing his Fellowship of the Royal Australasian College of Surgeons (FRACS) in Plastic Surgery in 2013, Dr Mistry relocated to Newcastle with his family in 2015. He began his work as a Visiting Medical Officer (VMO) in Plastic and Hand Surgery at John Hunter Hospital before establishing his private practice in 2017. His practice offers a comprehensive range of reconstructive and aesthetic procedures for the breast, body, face, and skin.
Dr Mistry’s approach to patient care is grounded in trust, respect, and open communication. From initial consultation to recovery, he aims to ensure patients feel informed, supported, and comfortable throughout their surgical journey. He is dedicated to maintaining the highest professional and ethical standards in all aspects of his work.
To remain at the forefront of modern surgical techniques, Dr Mistry continues to pursue ongoing professional development both in Australia and internationally. He was Australia’s first delegate at the Body Contouring Academy in Paris, where he received advanced training in body contouring and skin-tightening techniques, including VASER and RENUVION technologies.
Professional Memberships:
Fill in your details and our friendly team will be in touch with you
Please Note: Information provided on Dr Mistry’s website is provided as a basic guide, it does not constitute a diagnosis and should not be taken as medical advice. Any surgical or invasive procedure carries risks.





“I care because it’s my job as a surgeon, as a plastic surgeon, to do the appropriate thing and to give you a good outcome. I want to leave knowing that I can tell a patient, hand on heart, that I did the very best I could and that I looked after them, so when I see them post op later that day or the next morning, that they feel they were in good hands.”
– Dr Yezdi Mistry
Request a Consult