Gynaecomastia is a recognised medical condition involving an increase in glandular breast tissue in males. It may occur at different stages of life and can develop gradually. Many men find it difficult to discuss changes in the chest, and as a result, they often adapt clothing, activity patterns and daily routines to reduce attention to the area. Men who attend consultations in Charlestown frequently describe how long they managed these changes quietly before seeking an assessment.
This article outlines how men commonly hide gynaecomastia and why these behaviours develop. The aim is to provide clear and medically accurate information that aligns with AHPRA guidelines. The content is general and does not replace a personalised assessment. Individuals who notice persistent changes in the chest should seek professional medical evaluation.
Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon based in Charlestown, NSW. His approach is grounded in patient centred care, supported by specialist training and clinical experience.
Gynaecomastia involves enlargement of glandular tissue beneath the nipple. It is different from chest changes caused by adiposity alone, although some individuals experience a combination of both. Factors contributing to gynaecomastia may include hormonal shifts, medications, underlying health conditions or physiological changes that occur during adolescence or adulthood. In some situations, the reason remains unknown.
The degree of glandular enlargement varies between individuals. In some cases, it may be subtle but still noticeable in fitted clothing or certain lighting. Others experience a more significant change in the shape of the chest. Research shows that personal concern does not always correspond to the degree of enlargement. A person with mild changes may experience ongoing discomfort in social environments, while another person with more prominent changes may only feel aware of it occasionally.
Many men who attend consultations in Charlestown explain that they first observed changes during adolescence. Over time, they adapted their clothing and posture or adjusted their activities. Others first noticed changes during adulthood, often related to weight variation, medication use or hormonal factors. Research supports these patterns and describes how individuals often modify their routines to manage awareness of chest differences.


Men use a variety of strategies to reduce the appearance of gynaecomastia, and these habits can become part of daily life. Some develop these behaviours during adolescence, while others adopt them later.
Clothing adaptations are among the most common. Many men choose looser garments to reduce visible chest prominence. Layering is frequently used, such as wearing a T-shirt over a compression singlet or choosing thicker fabrics throughout the year. Dark colours and structured fabrics may also be selected to reduce shadows or outlines. Although these adjustments provide reassurance, they may limit comfort during warmer months in Newcastle and Lake Macquarie.
Postural changes develop gradually. Men may lean slightly forward, fold their arms across their chest or maintain standing positions that reduce visibility. These changes often occur without conscious awareness and can contribute to tension across the shoulders and neck.
Avoiding environments where the chest is more visible is another common pattern. Beaches, ocean baths, lakes, surf clubs, gyms and sports changing areas are frequently mentioned. Some men modify routines so they visit these places at quieter times. Others avoid them altogether. Clothing requirements for certain sports or activities may also influence participation.
In private settings, some men continue to use clothing to manage visibility, including at home or in shared living arrangements. These habits can influence comfort, movement and social interactions across many aspects of daily life.
These strategies do not indicate weakness. They are understandable responses to a physical change that some individuals find difficult to discuss. Recognising these behaviours allows men to understand that they are not alone and that these patterns are common.
The reasons behind concealment are influenced by social expectations, personal identity and external perceptions of male physical appearance. Research provides insight into why many men adopt these behaviours.
One key factor relates to common assumptions about the male chest. In many cultures, a flat chest is viewed as typical for men. When glandular tissue increases, some individuals feel that this creates an appearance that is different from what they believe is socially expected. Adolescence is a particularly sensitive period. Physical changes during this time can influence self perception, and concern about peer judgement is common.
Men often worry about misunderstanding. Some fear that others may assume the chest change is due to weight, steroid use or other health conditions. Others are concerned about unwanted questions or comments. These possibilities may make social environments feel unpredictable, leading individuals to adapt clothing or behaviour to reduce attention.
Body image is another reason. Although body image discussions often focus on women, research shows that many men also experience social and internal pressures regarding physical appearance. Fitness environments, social media and public imagery can contribute to comparison. Men with gynaecomastia may notice differences between their chest and what is commonly portrayed, which influences concealment.
Some individuals feel unsure about raising the topic with their GP or a specialist. They may feel embarrassed, uncertain about whether the issue is medically relevant or assume that options are limited. These hesitations are well documented and contribute to delayed help seeking.
Men who develop gynaecomastia due to medical treatments, including hormonal therapy for prostate conditions, may experience additional concerns. These changes may be linked with feelings about health or identity. These reactions vary and highlight the importance of supportive medical communication.
Understanding these factors helps men recognise that these behaviours are common responses to physical changes rather than personal shortcomings.
Long term concealment can influence physical, social and emotional aspects of everyday life. Not everyone is affected in the same way, but certain patterns appear frequently.
Clothing restrictions may reduce comfort, especially in the warm climate of Newcastle and the Hunter Region. Wearing multiple layers or heavier fabrics throughout the year may limit clothing options.
Avoidance of water based activities can prevent individuals from participating in swimming, surfing or other coastal recreation. This can reduce opportunities for social engagement, exercise and leisure.
Postural adaptations such as hunching or folding the arms can contribute to muscular tension or limit natural movement patterns. These changes may persist even after men gain more understanding of the condition, because the habits become familiar.
Some men gradually reduce involvement in group activities, exercise programs or social events that involve clothing changes or shirtless environments. These changes are often subtle but accumulate over time, influencing overall lifestyle patterns. Research indicates that persistent gynaecomastia can be associated with emotional strain in some individuals, particularly adolescents. This does not affect everyone, but it demonstrates how the condition can influence wellbeing in certain contexts.
Understanding these patterns may help individuals recognise how gynaecomastia has shaped their behaviour and whether they may benefit from discussing options with a medical practitioner.
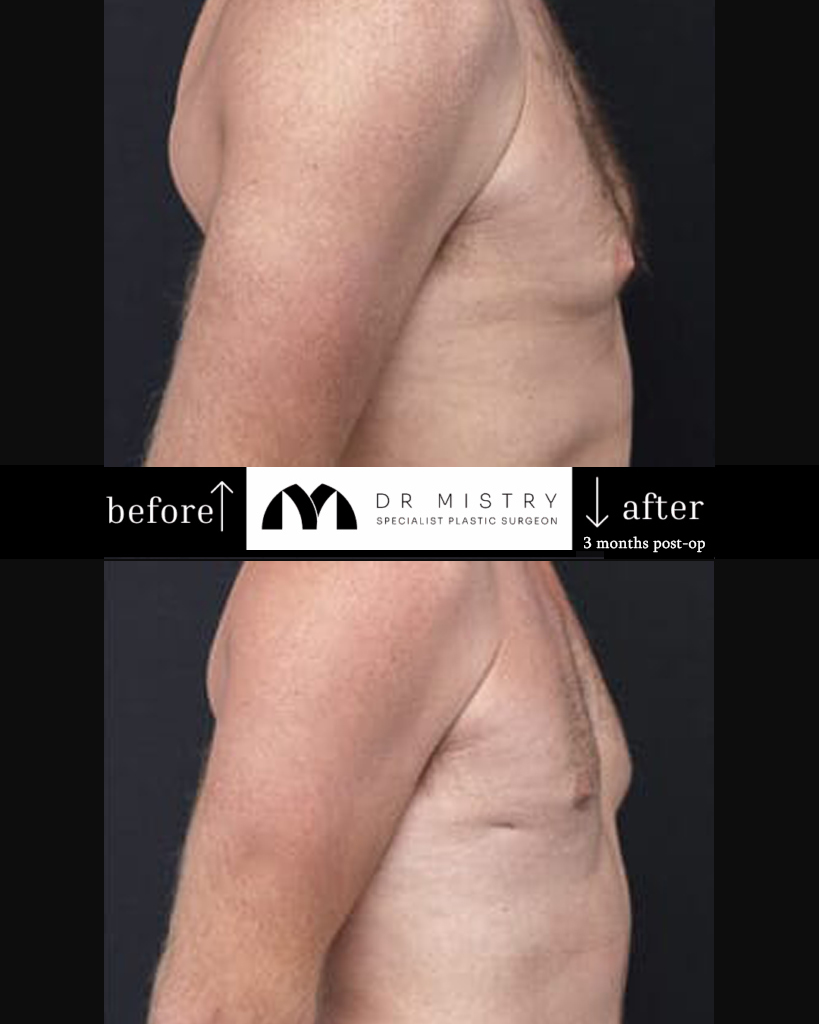
Disclaimer: The outcomes shown are specific to those patients and may not reflect the results experienced by others, as individual outcomes can vary due to a range of factors.


Seeking an assessment for gynaecomastia is a personal decision. Some individuals request advice early, while others delay for extended periods. An assessment does not mean that treatment is required. Instead, it provides clarity about the cause and options for management.
Men in Newcastle and the surrounding region often seek assessment when chest changes affect clothing options, daily movement, exercise routines or social comfort. Others want to clarify whether the change is related to glandular tissue, adiposity or a combination.
During a consultation with a GP or with a Specialist Plastic and Reconstructive Surgeon such as Dr Mistry in Charlestown, the assessment may include a medical history, physical examination and discussion of contributing factors. In some cases, additional investigations may be recommended. The goal is to provide information that supports informed decision making.
Depending on the cause, management may involve surgical or non surgical pathways. Any surgical or invasive procedure carries risks, and these are discussed carefully during consultation. A gradual recovery should be expected, and timelines vary between individuals. Treatment outcomes differ depending on anatomy, health and other personal factors.
Some men find that gaining clear information is enough to support their needs. Others may consider treatment after understanding the likely recovery process and the practical considerations involved. The most suitable approach depends on each person.
Patient centred care is an important part of managing gynaecomastia. It involves understanding the individual’s experience, concerns, expectations and lifestyle. This approach recognises that each person’s situation is influenced by different factors.
During consultations in Charlestown, Dr Mistry draws on his specialist training, clinical experience and years of practising in the region to support detailed assessments. Discussions focus on clarifying the condition, exploring management pathways and addressing practical requirements such as recovery expectations and activity planning.
For individuals who have concealed the condition for years, addressing established habits such as posture or activity avoidance may form part of ongoing support. Patient centred discussions help men understand the condition more clearly and make decisions that align with their circumstances.
Some men notice that the chest appears more prominent at certain times due to posture, lighting or fluid changes in the body. These variations do not necessarily indicate progression. A medical assessment can help clarify what contributes to these changes.
Yes, unilateral gynaecomastia can occur. This can make the change feel more noticeable, even when the glandular tissue is mild. An examination helps determine whether the difference is due to glandular tissue, adiposity or another factor.
Exercise can support general health and influence fat distribution, but it does not reduce established glandular breast tissue. Some men notice improved comfort with strength training, while others find the appearance unchanged. A clinician can help identify the type of tissue involved.
Yes, although many choose not to because of awareness of chest visibility. Some adjust clothing or select quieter times at local beaches and pools. Understanding the condition may help individuals decide how they want to approach these settings.
No. Some men prefer monitoring once they understand the cause, while others consider treatment based on their individual circumstances. The most suitable approach depends on anatomy, medical factors and personal priorities.
Certain medications may influence hormonal balance, which can contribute to glandular enlargement in some individuals. If medication is a suspected factor, a GP can review options and advise whether adjustments are appropriate. A specialist assessment may also be recommended.
Yes, delayed help seeking is frequently described in medical research and is common in clinical practice. Many men adapt their routines for years before feeling ready to raise the concern. An initial consultation can provide clarity even if no treatment is pursued.
Weight loss may reduce adipose tissue in the chest, which can make underlying glandular tissue appear more defined. This does not mean the condition is worsening. An assessment can help distinguish between fat reduction and glandular tissue.
Yes, some men notice a visible change without any physical symptoms. Others may experience sensitivity in the area, particularly during periods of hormonal fluctuation. Both presentations are recognised patterns seen in clinical practice.
Posture can influence the way the chest looks. Some individuals adopt protective postures over time, which can further change the appearance. A clinician can explain how posture interacts with glandular or adipose tissue in the chest.
Charlestown, Newcastle and Lake Macquarie have a strong outdoor lifestyle culture. Beaches, lakefronts, walking tracks, surf clubs and community gyms are common parts of daily life. In these environments, clothing is often minimal, which can heighten awareness of gynaecomastia.
Men who attend Dr Mistry’s practice frequently explain how they modified their routines. Examples include wearing a T shirt during swimming, avoiding certain sports, selecting gym times with fewer people present or choosing clothing that does not reflect the climate simply to reduce attention to the chest.
Having access to a Specialist Plastic and Reconstructive Surgeon within Charlestown allows men across the Hunter Region to discuss their concerns without needing to travel. Many describe feeling relieved once they understand the condition clearly and have an opportunity to discuss options in a private and supportive environment.
Gynaecomastia can influence many areas of life, especially when concealment becomes an ongoing pattern. Understanding how these behaviours develop and what options may be available provides individuals with a basis for informed decisions. Some men find that assessment and information are enough to support them. Others may consider treatment based on their personal situation.
Any surgical or invasive procedure carries risks, and outcomes vary between individuals. Recovery progresses gradually, and treatment requires planning. Dr Mistry’s role as a Specialist Plastic and Reconstructive Surgeon is to provide information supported by established clinical training and to guide patients through their options with clarity and transparency.
Gynaecomastia is more common than many realise. The behaviours men use to manage visibility of the chest often develop gradually and are shared by many individuals. Recognising these patterns can help reduce feelings of isolation.
Men in Charlestown, Newcastle and the broader Hunter Region who have experienced persistent chest enlargement or long term concealment habits may find an assessment helpful. Dr Yezdi Mistry provides individualised consultations informed by specialist training and professional experience. Anyone considering an evaluation is encouraged to seek medical advice to gain a clearer understanding of their situation.

Dr Yezdi Mistry is a Specialist Plastic and Reconstructive Surgeon based in Newcastle, NSW. With extensive training and experience in both reconstructive and aesthetic surgery, Dr Mistry is committed to providing safe, evidence-based care that is tailored to each patient’s individual needs.
After completing his Fellowship of the Royal Australasian College of Surgeons (FRACS) in Plastic Surgery in 2013, Dr Mistry relocated to Newcastle with his family in 2015. He began his work as a Visiting Medical Officer (VMO) in Plastic and Hand Surgery at John Hunter Hospital before establishing his private practice in 2017. His practice offers a comprehensive range of reconstructive and aesthetic procedures for the breast, body, face, and skin.
Dr Mistry’s approach to patient care is grounded in trust, respect, and open communication. From initial consultation to recovery, he aims to ensure patients feel informed, supported, and comfortable throughout their surgical journey. He is dedicated to maintaining the highest professional and ethical standards in all aspects of his work.
To remain at the forefront of modern surgical techniques, Dr Mistry continues to pursue ongoing professional development both in Australia and internationally. He was Australia’s first delegate at the Body Contouring Academy in Paris, where he received advanced training in body contouring and skin-tightening techniques, including VASER and RENUVION technologies.
Professional Memberships:
Fill in your details and our friendly team will be in touch with you
Please Note: Information provided on Dr Mistry’s website is provided as a basic guide, it does not constitute a diagnosis and should not be taken as medical advice. Any surgical or invasive procedure carries risks.





“I care because it’s my job as a surgeon, as a plastic surgeon, to do the appropriate thing and to give you a good outcome. I want to leave knowing that I can tell a patient, hand on heart, that I did the very best I could and that I looked after them, so when I see them post op later that day or the next morning, that they feel they were in good hands.”
– Dr Yezdi Mistry
Request a Consult